Benzodiazepine Addiction: Signs, Symptoms, and Treatment Options
Discover benzodiazepine addiction signs, withdrawal symptoms, and proven treatment options. Learn how to recognize dependence and find effective recovery paths.

Benzodiazepine addiction has become a growing concern in modern healthcare, affecting millions of people who initially sought relief from anxiety, insomnia, or panic disorders. These prescription medications, including popular brands like Xanax, Valium, and Klonopin, work by enhancing the brain’s GABA activity to produce calming effects. While effective for short-term use, benzodiazepines carry a high risk of physical and psychological dependence that can develop in as little as a few weeks of regular use.
Understanding the signs and symptoms of benzodiazepine addiction is the first step toward recovery. Many people don’t realize they’ve developed a dependency until they experience withdrawal symptoms when trying to reduce or stop their medication. The challenge lies in distinguishing between therapeutic use and problematic abuse, especially when these drugs are prescribed by doctors for legitimate medical conditions.
This comprehensive guide explores the warning signs of benzo addiction, explains how dependence develops, details the often-dangerous withdrawal process, and outlines evidence-based treatment options that can help you or a loved one break free from benzodiazepine dependence. Whether you’re concerned about your own use or worried about someone close to you, understanding this addiction is crucial for making informed decisions about treatment and recovery.
Understanding Benzodiazepines and How Addiction Develops
What Are Benzodiazepines?
Benzodiazepines are a class of central nervous system depressants commonly prescribed to treat anxiety disorders, panic attacks, seizures, muscle spasms, and insomnia. These medications work by binding to GABA receptors in the brain, which are responsible for inhibiting neural activity and producing calming, sedative effects. Common benzodiazepines include alprazolam (Xanax), diazepam (Valium), lorazepam (Ativan), clonazepam (Klonopin), and temazepam (Restoril).
According to research, approximately 30.5 million people in the United States used benzodiazepines between 2015 and 2016, with about 15% of adults taking these medications at some point during the year. While they can provide immediate relief from distressing symptoms, their effectiveness comes with significant risks when used beyond short-term treatment periods.
The Path from Prescription to Addiction
The journey to benzodiazepine addiction often begins innocently with a legitimate prescription. Here’s how physical dependence typically develops:
- Initial therapeutic use: A doctor prescribes benzodiazepines for anxiety, panic disorder, or insomnia
- Tolerance development: The brain adapts to the drug’s presence, requiring higher doses to achieve the same effects
- Increased dosage: Users take more medication than prescribed or use it more frequently
- Physical dependence: The body requires the drug to function normally
- Addiction: Compulsive drug-seeking behavior develops despite negative consequences
The development of tolerance is a natural physiological process that occurs when the brain’s chemistry adjusts to the consistent presence of the drug. Every person’s body chemistry is different, so the timeline for developing benzodiazepine dependence varies significantly. Some individuals may develop dependence within a few weeks of daily use, while others may take months or even years.
Risk Factors for Benzodiazepine Addiction
Several factors increase the likelihood of developing benzodiazepine addiction:
- Long-term use beyond four weeks
- Use of high-potency, short-acting benzodiazepines like Xanax
- Personal or family history of substance use disorder
- Pre-existing mental health disorders such as anxiety or depression
- High-stress environments or traumatic life events
- Easy access to the medication
- Previous issues with alcohol or drug dependency
- Female gender (women are prescribed benzodiazepines at higher rates)
Research from the Drug Enforcement Administration indicates that approximately 5.2 million adults misuse these medications, with around 15% of those prescribed benzodiazepines developing an addiction.
Recognizing the Signs and Symptoms of Benzodiazepine Addiction
Physical Signs of Benzo Abuse
Benzodiazepine addiction manifests through various physical symptoms that become more pronounced over time. Being able to identify these warning signs can be lifesaving:
Common physical symptoms include:
- Drowsiness and excessive sedation during daytime hours
- Slurred speech and difficulty articulating thoughts
- Poor coordination and impaired motor skills
- Blurred vision and dizziness
- Tremors or shaking, particularly in the hands
- Muscle weakness and fatigue
- Headaches and confusion
- Changes in appetite and weight fluctuations
- Respiratory depression (slowed breathing)
- Memory problems and cognitive impairment
When benzodiazepines are combined with other central nervous system depressants like alcohol or opioids, the physical risks multiply dramatically. This dangerous combination can lead to respiratory depression, unconsciousness, and even death.
Behavioral Warning Signs
The behavioral changes associated with benzodiazepine addiction often affect relationships, work performance, and daily responsibilities:
- Doctor shopping: Seeking prescriptions from multiple physicians to obtain more medication
- Obsessive focus on securing and using the drug
- Neglecting work, school, or family obligations
- Social withdrawal and isolation from friends and family
- Loss of interest in previously enjoyed activities
- Taking larger doses than prescribed
- Running out of prescriptions early
- Engaging in risky behaviors while under the influence
- Defensive or secretive behavior about medication use
- Continuing use despite negative consequences
According to the Substance Abuse and Mental Health Services Administration, recognizing these behavioral patterns early can significantly improve treatment outcomes.
Psychological and Emotional Symptoms
Benzodiazepine abuse significantly impacts mental health and emotional well-being:
- Increased anxiety and panic attacks (ironically, the conditions being treated)
- Depression and persistent feelings of sadness
- Mood swings and emotional instability
- Irritability and heightened aggression
- Intense cravings for the medication
- Feeling unable to cope without the drug
- Cognitive difficulties including confusion and impaired judgment
- Concentration problems and memory lapses
- Emotional numbness or detachment
- Heightened emotional distress
Many individuals with mental health conditions face a particularly challenging situation, as they may have started taking benzodiazepines to manage legitimate symptoms. The line between therapeutic use and addiction becomes blurred, creating a cycle of dependence that’s difficult to recognize and even harder to break without professional intervention.
The Dangerous Reality of Benzodiazepine Withdrawal
Why Benzo Withdrawal Is Life-Threatening
Benzodiazepine withdrawal is considered one of the most dangerous types of drug withdrawal, alongside alcohol withdrawal. Unlike many other substances, abruptly stopping benzodiazepines can be fatal. This is why medical detox under professional supervision is absolutely essential for anyone dependent on these medications.
When you suddenly stop taking benzodiazepines, the brain’s GABA receptors, which have adapted to the drug’s presence, become hyperactive. This creates an overall state of excessive nervous system excitation, leading to potentially life-threatening complications.
Timeline of Benzodiazepine Withdrawal
The withdrawal timeline varies based on whether you’ve been taking short-acting or long-acting benzodiazepines:
Early Withdrawal Phase (6-24 hours for short-acting, 1-3 days for long-acting)
- Return of anxiety and insomnia symptoms
- Mild irritability and restlessness
- Initial discomfort and muscle stiffness
- Rebound symptoms (return of original symptoms)
Peak Withdrawal Phase (Days 1-14)
- Severe anxiety and panic attacks
- Hand tremors and shaking
- Profuse sweating
- Nausea and vomiting
- Difficulty concentrating
- Confusion and cognitive difficulties
- Memory problems
- Muscle pain and stiffness
- Headaches
- Palpitations
- Sleep disturbances
- Seizures (potentially life-threatening)
- Hallucinations
- Psychotic reactions
Protracted Withdrawal (Weeks to Months) Approximately 10-15% of individuals experience what’s known as Post-Acute Withdrawal Syndrome (PAWS), which can persist for months or even years. Symptoms include:
- Persistent anxiety and mood swings
- Prolonged insomnia
- Cognitive deficits
- Depression
- Tingling in extremities
- Muscle twitches
- Random fluctuations in symptoms
Common Withdrawal Symptoms
According to research published in psychiatric journals, approximately 40% of individuals who have taken benzodiazepines longer than six months will experience moderate to severe withdrawal symptoms. These include:
- Anxiety and increased tension
- Panic attacks
- Tremors and shaking
- Sweating and hot/cold flashes
- Difficulty sleeping (insomnia)
- Irritability and mood swings
- Concentration problems
- Confusion and memory issues
- Nausea and digestive problems
- Headaches
- Muscle pain and stiffness
- Sensory disturbances
- Depersonalization (feeling detached from reality)
- Depression
- Suicidal thoughts or ideation
- Seizures (in severe cases)
The National Institute on Drug Abuse emphasizes that withdrawal symptoms can be minimized through proper medical detox protocols and gradual tapering under medical supervision.
Comprehensive Treatment Options for Benzodiazepine Addiction
Medical Detoxification: The Critical First Step
Medical detox is the safest and most effective way to begin recovery from benzodiazepine addiction. Unlike many other substances where “cold turkey” cessation is uncomfortable but not dangerous, stopping benzodiazepines abruptly can trigger seizures, severe psychological distress, and potentially fatal complications.
Key components of medical detox include:
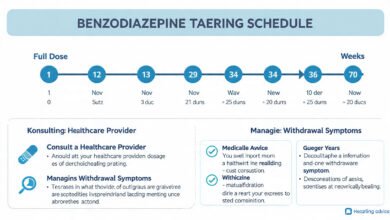
- Gradual tapering: Slowly reducing the dosage over weeks or months to minimize withdrawal symptoms
- 24/7 medical supervision: Continuous monitoring of vital signs and symptoms
- Medication-assisted treatment: Using longer-acting benzodiazepines like diazepam (Valium) to ease withdrawal
- Symptom management: Addressing specific withdrawal effects as they arise
- Safe environment: Removal from temptation and triggers that might cause relapse
The tapering process typically involves switching from a short-acting benzodiazepine to a longer-acting one with a more gradual offset. This substitution helps prevent the interdose withdrawal and rebound effects that make short-acting benzodiazepines particularly difficult to discontinue.
Inpatient vs. Outpatient Treatment
Inpatient Treatment (Residential Rehab)
Inpatient programs provide the highest level of care and are recommended for:
- Individuals with severe benzodiazepine addiction
- Those with a history of failed outpatient attempts
- People with co-occurring mental health disorders
- Those lacking a stable support system
- Individuals at high risk for complications
Benefits include:
- Round-the-clock medical supervision
- Structured therapeutic environment
- Removal from triggers and stressors
- Comprehensive dual diagnosis treatment
- Intensive therapy and counseling
- Duration typically ranges from 30 to 90 days
Outpatient Treatment
Outpatient programs work well for:
- Mild to moderate addiction
- Strong home support systems
- Work or family obligations that cannot be paused
- Those who have completed inpatient treatment
Outpatient services include:
- Regular therapy sessions
- Medical monitoring
- Support group participation
- Flexible scheduling around daily responsibilities
Evidence-Based Therapeutic Approaches
Cognitive Behavioral Therapy (CBT)
Cognitive behavioral therapy has proven to be one of the most effective treatments for benzodiazepine addiction. Research shows success rates between 70-80% when CBT is combined with gradual dose reduction. CBT helps individuals:
- Identify triggers and patterns that lead to drug use
- Develop healthy coping strategies for anxiety and stress
- Challenge distorted thinking patterns
- Build skills to prevent relapse
- Address underlying anxiety disorders without medication
Additional Therapeutic Modalities:
- Individual counseling for personalized treatment
- Group therapy for peer support and shared experiences
- Family therapy to repair relationships and build support systems
- Mindfulness and relaxation techniques
- Dialectical behavior therapy (DBT) for emotional regulation
- Motivational interviewing to strengthen commitment to recovery
Medication-Assisted Treatment
While the goal is to eliminate benzodiazepine use, certain medications can support the withdrawal and recovery process:
- Longer-acting benzodiazepines: Used during tapering to prevent severe withdrawal
- Flumazenil: A GABA receptor antagonist that may help reduce withdrawal severity (used in specialized settings only)
- Pregabalin: May help reduce withdrawal symptoms and relapse risk
- Antidepressants: For managing co-occurring depression (though SSRIs show limited effectiveness for benzodiazepine-related depression)
- Buspirone: A non-addictive anti-anxiety medication
Treatment Duration and Long-Term Recovery
The duration of benzodiazepine addiction treatment varies significantly based on individual factors:
- Medical detoxification: Typically 7-14 days, though tapering may take weeks to months
- Residential inpatient treatment: Usually 30-90 days
- Outpatient therapy: Several months to over a year
- Ongoing support: Lifetime commitment to recovery maintenance
Studies demonstrate that gradual dose reduction combined with psychological treatment is superior to medication tapering alone. A meta-analysis found that adding cognitive behavioral therapy during the taper significantly improved outcomes compared to dose reduction without therapy.
Addressing Co-Occurring Mental Health Disorders
The Complex Relationship Between Mental Health and Benzo Addiction
Approximately 7.4% of patients in psychiatric care are prescribed benzodiazepines, creating a challenging intersection between treating mental health disorders and preventing addiction. Many individuals initially receive these medications for legitimate conditions such as:
- Generalized anxiety disorder (GAD)
- Panic disorder
- Social anxiety disorder
- Post-traumatic stress disorder (PTSD)
- Insomnia
- Depression with anxiety symptoms
The paradox is that while benzodiazepines provide immediate symptom relief, long-term use can actually worsen the underlying mental health condition. Research indicates that prolonged benzodiazepine use carries a significant risk of causing depression, with studies showing that individuals who used benzodiazepines long-term developed depression at higher rates than those who used other substances.
Dual Diagnosis Treatment
Dual diagnosis treatment addresses both substance use disorder and mental health disorders simultaneously. This integrated approach is essential because:
- Untreated mental health issues increase relapse risk
- Addiction symptoms can mask or mimic psychiatric disorders
- Both conditions influence each other’s severity and progression
- Recovery requires treating the whole person, not just the addiction
Effective dual diagnosis treatment includes:
- Comprehensive psychiatric evaluation
- Individualized treatment plans addressing both conditions
- Medication management for mental health (using non-addictive alternatives)
- Specialized therapy targeting co-occurring disorders
- Long-term monitoring and support
Prevention and Risk Reduction Strategies
Safe Prescribing Practices
Healthcare providers can reduce the risk of benzodiazepine dependence through:
- Limiting prescriptions to 1-2 weeks supply
- Prescribing the lowest effective dose
- Regular monitoring of patients on long-term treatment
- Educating patients about addiction risks
- Exploring non-pharmacological alternatives first
- Considering less addictive medications when appropriate
Alternative Treatment Approaches
For anxiety disorders and insomnia, non-pharmacological treatments often prove more effective long-term:
- Cognitive behavioral therapy for insomnia (CBT-I)
- Exposure therapy for anxiety disorders
- Mindfulness-based stress reduction
- Regular exercise and physical activity
- Sleep hygiene improvements
- Relaxation techniques and meditation
- Biofeedback and neurofeedback
- Dietary modifications and nutritional support
Research shows that cognitive behavioral therapy is more effective than sedative hypnotic drugs for long-term management of insomnia, with success rates between 70-80%.
Getting Help: Resources and Next Steps
When to Seek Professional Help
You should consider professional treatment for benzodiazepine addiction if you experience:
- Increasing tolerance requiring higher doses
- Withdrawal symptoms when reducing or stopping use
- Unsuccessful attempts to cut down or quit
- Medication use affecting work, relationships, or responsibilities
- Strong cravings or inability to control use
- Spending considerable time obtaining, using, or recovering from the drug
- Continuing use despite knowing it causes harm
- Taking medication longer or in higher amounts than prescribed
Finding Treatment Services
If you or someone you care about is struggling with benzodiazepine addiction, several resources can help:
- SAMHSA National Helpline: 1-800-662-HELP (4357) – Free, confidential, 24/7 support and treatment referrals
- Primary care physician: Can provide referrals to addiction specialists
- Addiction treatment facilities: Offer specialized benzodiazepine recovery programs
- Mental health professionals: Can address co-occurring disorders
- Support groups: Provide peer support and shared experiences
Insurance and Financial Considerations
Many insurance plans cover substance use disorder treatment, including:
- Medical detoxification
- Inpatient rehabilitation
- Outpatient therapy
- Medication-assisted treatment
For those without insurance or with limited coverage, options include:
- State-funded treatment programs
- Sliding-scale payment programs
- Community health centers
- SAMHSA treatment locator for affordable options
Conclusion
Benzodiazepine addiction represents a serious but treatable condition that affects millions of people who initially sought legitimate medical treatment. Understanding the signs and symptoms of benzo addiction, recognizing the dangers of withdrawal, and knowing that effective treatment options exist are crucial first steps toward recovery. While benzodiazepines serve important therapeutic purposes for short-term use, the risks of physical dependence and addiction necessitate careful prescribing practices and patient education. If you’re struggling with benzodiazepine dependence, remember that recovery is possible through comprehensive treatment that includes medical detox, evidence-based therapies like cognitive behavioral therapy, and ongoing support for co-occurring mental health disorders. The journey may be challenging, but with proper professional help, you can safely withdraw from benzodiazepines and rebuild a healthier life free from addiction.