Xanax vs Valium Addiction: Key Differences Explained
Xanax vs Valium addiction explained: discover 7 critical differences in dependency risk, withdrawal severity, half-life, and how to get effective treatment today.
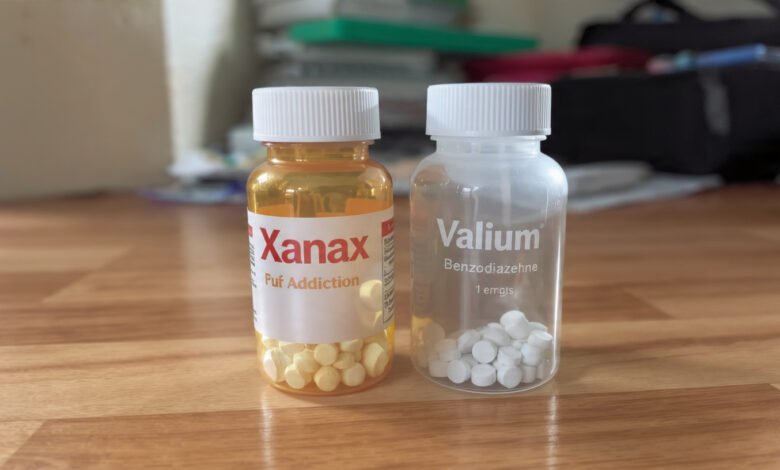
Xanax vs Valium addiction is one of the most searched topics in prescription drug recovery — and for good reason. These two medications are among the most widely prescribed drugs in the United States, yet most people have no idea how differently they behave inside the body, especially when misuse or dependence enters the picture.
Both Xanax (alprazolam) and Valium (diazepam) belong to a class of drugs called benzodiazepines. They both calm the central nervous system, reduce anxiety, and carry a real risk of physical dependence. But the similarities start to break down pretty fast once you dig deeper.
The differences in their half-life, onset of action, abuse potential, and withdrawal severity are not minor. They shape everything — how quickly someone gets hooked, how intense the detox process is, and what kind of treatment approach works best.
If you or someone you care about is taking either of these medications, or if you are trying to understand a developing dependency, this guide lays out everything clearly. This is not medical advice, but it is an honest, research-backed look at what makes these two drugs different — and why those differences matter enormously when it comes to benzodiazepine addiction and recovery.
What Are Xanax and Valium?
Before getting into the differences, it helps to understand what each drug actually is and what it is prescribed for.
Xanax (Alprazolam)
Xanax is the brand name for alprazolam, a short-acting benzodiazepine. The U.S. Food and Drug Administration (FDA) has approved it to treat:
- Generalized anxiety disorder (GAD)
- Panic disorder, including agoraphobia
Xanax is only available in oral tablet form. Because of its potency and short duration, doctors generally limit its use to acute anxiety or panic episodes. It is classified as a Schedule IV controlled substance by the Drug Enforcement Administration (DEA), meaning it has recognized medical uses but also a real potential for abuse and dependence.
Valium (Diazepam)
Valium is the brand name for diazepam, a long-acting benzodiazepine. It has a broader range of approved uses than Xanax, including:
- Anxiety disorders
- Alcohol withdrawal symptoms
- Seizure disorders and epilepsy
- Muscle spasms
- Procedural sedation
Valium is also a Schedule IV drug. It has been around since the 1960s and remains one of the most prescribed medications globally. Its longer-lasting effects make it useful for more medical conditions than Xanax, but it comes with its own risks when used beyond prescription guidelines.
How Both Drugs Work
Both alprazolam and diazepam work by enhancing the activity of GABA (gamma-aminobutyric acid), the brain’s primary inhibitory neurotransmitter. GABA slows down neuronal activity — which is why these drugs reduce anxiety, prevent seizures, relax muscles, and induce sleep. When benzodiazepines bind to GABA-A receptors, they make GABA’s calming effects far more powerful than they would be naturally.
This mechanism is also why benzodiazepine dependence develops — the brain starts to rely on the drug to maintain normal GABA function, and it stops producing GABA as effectively on its own.
Xanax vs Valium Addiction: 7 Critical Differences
1. Half-Life: The Biggest Structural Difference
The half-life of a drug is the time it takes for the body to eliminate half of it from the bloodstream. This single factor shapes nearly everything about how addictive a benzodiazepine is.
- Xanax half-life: approximately 11–12 hours
- Valium half-life: approximately 20–70 hours, with active metabolites that can extend effects up to 100+ hours in some individuals
What does this mean in practice? Xanax leaves your system much faster. When a drug exits the body quickly, the brain notices its absence sooner — which triggers withdrawal symptoms earlier and more intensely. This rapid “on-off” cycle is a major driver of Xanax addiction, because users often feel compelled to take another dose just to ward off the discomfort of early withdrawal.
Valium’s long half-life means the drug tapers out of the system more gradually, which tends to make withdrawal slower to start and — in many cases — less acutely severe. However, Valium withdrawal can still be dangerous and drawn-out if the dependency is deep.
2. Addiction Risk and Abuse Potential
Research consistently shows that Xanax carries a higher abuse potential than Valium. There are several reasons for this:
- Its faster onset of action produces a more immediate and intense calming effect, which reinforces the urge to take more
- Its shorter half-life means the pleasurable effects wear off quickly, leading users to redose more frequently
- Gram for gram, alprazolam is more potent than diazepam — meaning smaller doses produce stronger effects
In smaller doses, Xanax is more powerful than Valium and is more likely to cause tolerance or physical dependence.
Research suggests that Xanax has a higher risk of physical dependence and addiction than Valium.
This does not mean Valium is safe to misuse. Valium addiction is absolutely real and can develop after weeks of consistent use. But the risk curve is steeper and faster with Xanax.
3. Speed of Dependence Development
Physical dependence — meaning the body adapts to the drug and requires it to function normally — can develop with both medications, but the timeline differs.
With Xanax, dependence can develop in as little as a few weeks of daily use, particularly at higher doses. Some clinical sources report signs of dependence appearing within days in people with certain risk factors.
With Valium, dependence still develops relatively quickly by pharmaceutical standards, but the process tends to unfold over a slightly longer timeline due to the drug’s gradual accumulation in the body. Because Valium builds up slowly, some users may not realize they are dependent until they try to stop.
Key risk factors that accelerate dependence with either drug include:
- Taking higher doses than prescribed
- Using the drug daily rather than as needed
- Combining benzodiazepines with alcohol or opioids
- A personal or family history of substance use disorder
- Using the medication longer than prescribed
4. Withdrawal Symptoms: Xanax vs Valium
Benzodiazepine withdrawal is one of the most dangerous withdrawal syndromes in all of addiction medicine — arguably more medically serious than opioid withdrawal. Both Xanax withdrawal and Valium withdrawal can include:
- Severe anxiety and panic attacks
- Insomnia
- Seizures (potentially life-threatening)
- Tremors and muscle cramps
- Sweating and heart palpitations
- Rebound anxiety — anxiety that is worse than before the drug was started
- Confusion and cognitive impairment
- In extreme cases, psychosis
The critical difference lies in timing and intensity:
Xanax withdrawal typically begins within 6–12 hours of the last dose. Because Xanax leaves the system so quickly, the nervous system reacts sharply and fast. Symptoms tend to be intense and can escalate to life-threatening seizures without medical supervision. A medical team often supervises Xanax withdrawals to ensure the least amount of side effects possible during detox.
Valium withdrawal usually begins more slowly — often 24–72 hours after the last dose — and can last much longer, sometimes weeks or months in cases of protracted withdrawal syndrome (PAWS). The drawn-out timeline can be exhausting, but the acute danger window is often less compressed than with Xanax.
Neither withdrawal process should be attempted without medical guidance. Cold turkey cessation from either drug can be fatal in severe cases.
5. Medical Uses and Prescription Patterns
The range of conditions each drug treats affects how and why people come to depend on them.
Xanax is prescribed more narrowly — primarily for anxiety and panic disorders. Because it hits fast and hard, it is often used for acute situations, like a panic attack or a high-stress event. The problem is that patients who take it for situational anxiety can quickly find themselves taking it daily “just to function.” That is where prescription drug dependence takes root.
Valium covers a much wider clinical territory. Doctors prescribe it for alcohol detox, epilepsy, muscle injury, and procedural anxiety. Because it stays in the body so long, it is sometimes intentionally used as a tapering drug during benzodiazepine withdrawal protocols — including for Xanax addiction. The irony is that a drug people become addicted to is also used to help people get off other benzodiazepines.
6. Overdose Risk
Both drugs carry a risk of overdose, particularly when combined with:
- Alcohol
- Opioids (this combination is extremely dangerous and responsible for a large number of overdose deaths)
- Other CNS depressants like sleeping pills or muscle relaxants
The overdose risk greatly increases when taking more than one type of benzo at a time. Benzodiazepine overdose is generally not fatal but can greatly increase the risk of death when mixed with other drugs, such as opioids.
Because Xanax is more potent per milligram and leaves the body faster (leading to redosing behavior), the overdose risk tends to be higher. Valium’s slower accumulation means toxic levels can build gradually without the user realizing it — especially in older adults whose liver metabolizes drugs more slowly.
Signs of benzodiazepine overdose that require immediate emergency care include:
- Extreme drowsiness or unconsciousness
- Slow, labored, or stopped breathing
- Blue-tinged lips or fingertips (cyanosis)
- Unresponsiveness
- Seizures
If you suspect a benzodiazepine overdose, call 911 immediately.
7. Treatment Approaches
Benzodiazepine addiction treatment is not one-size-fits-all, and the approach often differs based on whether the person is dependent on Xanax or Valium.
Xanax Addiction Treatment
Because Xanax withdrawal is so acute and fast-moving, treatment almost always begins with a medically supervised detox. Clinicians often use a controlled taper — sometimes switching the patient to a longer-acting benzodiazepine like Valium or Librium — to reduce the severity of withdrawal and prevent seizures.
After detox, comprehensive treatment typically includes:
- Cognitive Behavioral Therapy (CBT) to address anxiety triggers that originally drove the drug use
- Individual and group therapy
- Medication management if there is an underlying anxiety disorder
- Long-term relapse prevention planning
Valium Addiction Treatment
Valium addiction treatment follows a similar structure, though the detox phase can stretch over a longer period due to the drug’s extended half-life. A gradual dose reduction is standard practice. Because Valium is sometimes already the long-acting substitute used in tapers, clinicians carefully calibrate the pace of the taper to avoid protracted withdrawal.
Treatment programs that address both the physical and psychological components of benzo dependence give people the strongest chance of sustained recovery. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), evidence-based treatment for benzodiazepine use disorder includes therapy, peer support, and in many cases, dual diagnosis treatment for co-occurring mental health conditions.
Signs of Benzodiazepine Addiction to Watch For
Whether the drug is Xanax or Valium, addiction tends to follow recognizable patterns. Here are the warning signs that indicate a problem has developed:
- Increased tolerance — needing more of the drug to get the same effect
- Taking the drug more often or in higher doses than prescribed
- Doctor shopping — visiting multiple providers to obtain extra prescriptions
- Using the drug to cope with everyday stress, not just acute medical need
- Mood and behavior changes — irritability, social withdrawal, secretiveness
- Physical symptoms between doses — anxiety, sweating, tremors
- Failed attempts to cut down or stop
- Continued use despite negative consequences — relationship problems, work issues, health decline
If several of these signs sound familiar, it is worth talking to a healthcare provider or calling SAMHSA’s National Helpline at 1-800-662-4357 (free, confidential, 24/7).
Xanax vs Valium Addiction: Comparison Table
| Factor | Xanax (Alprazolam) | Valium (Diazepam) |
|---|---|---|
| Generic Name | Alprazolam | Diazepam |
| Drug Class | Benzodiazepine | Benzodiazepine |
| Half-Life | 11–12 hours | 20–70 hours |
| Onset of Action | 15–30 minutes | 15–60 minutes |
| Primary Uses | Anxiety, panic disorder | Anxiety, seizures, muscle spasms, alcohol withdrawal |
| Addiction Risk | Higher | Moderate-High |
| Withdrawal Onset | 6–12 hours after last dose | 24–72 hours after last dose |
| Withdrawal Severity | Intense, acute | Prolonged, can be drawn-out |
| DEA Schedule | Schedule IV | Schedule IV |
| Overdose Risk | High (especially with opioids/alcohol) | High (especially with opioids/alcohol) |
Common Myths About Xanax and Valium Addiction
Myth: “It’s prescribed, so it’s safe to take long-term.”
False. Prescription status means a drug has legitimate medical uses, not that long-term use is risk-free. Neither drug should be used regularly due to the potential for addiction. Both Valium and Xanax should be used short-term only.
Myth: “Valium is safer than Xanax.”
Partially false. Valium may have a slightly lower acute addiction risk, but “safer” is relative. Valium dependence is real and serious. The prolonged withdrawal from Valium can be just as challenging as Xanax — just in a different way.
Myth: “If I’m not taking it to get high, I can’t be addicted.”
False. Physical dependence develops based on how the brain adapts to the drug — not on intent. Many people who take benzodiazepines exactly as prescribed still develop dependency over time.
Myth: “I can quit cold turkey once I decide to stop.”
Dangerous and false. Stopping either drug abruptly after dependency has set in can trigger life-threatening seizures. Always consult a medical professional before discontinuing a benzodiazepine.
The Role of Co-Occurring Disorders
One of the most important and often overlooked aspects of benzodiazepine addiction is how frequently it occurs alongside other mental health conditions. Most people who are prescribed Xanax or Valium are dealing with real, diagnosed anxiety disorders, PTSD, depression, or panic disorder.
When addiction develops in this context, it creates a dual challenge: the person needs help with both the substance use disorder and the underlying mental health condition. Treating one without the other dramatically increases the risk of relapse.
This is why quality treatment programs offer dual diagnosis care — integrated treatment that addresses both issues simultaneously. The National Institute on Drug Abuse (NIDA) notes that people with anxiety disorders are at heightened risk for benzodiazepine misuse precisely because the drugs offer such immediate relief from symptoms that feel unbearable.
How to Get Help for Benzodiazepine Addiction
If you or someone close to you is struggling with Xanax addiction, Valium addiction, or benzo dependence more broadly, the most important step is reaching out. You do not have to navigate this alone, and you should not attempt detox without medical support.
Here are practical steps to take:
- Talk to your doctor honestly about your current use and any symptoms you have noticed
- Do not stop suddenly — always work with a provider on a taper schedule
- Contact a treatment center that specializes in benzodiazepine dependence
- Call SAMHSA’s helpline at 1-800-662-4357 for free, confidential referrals
- Consider dual diagnosis treatment if you have an underlying anxiety or mood disorder
- Build a support system — therapy, peer groups, and honest conversations with trusted people matter enormously in recovery
Recovery from benzodiazepine addiction is absolutely possible, and people do it every day. The key is getting the right kind of structured, medically sound support.
Conclusion
Xanax vs Valium addiction comes down to a set of meaningful clinical differences that directly impact how dependence develops, how severe withdrawal becomes, and what kind of treatment works best. Xanax (alprazolam) carries a higher abuse potential due to its short half-life and intense, fast-acting effects, while Valium (diazepam) poses its own serious risks through slower-developing but potentially prolonged dependence.
Both are Schedule IV controlled substances, both enhance GABA activity in the brain, and both can cause life-threatening withdrawal without proper medical supervision. Whether you are trying to understand a prescription you have been given, recognize the warning signs of dependency in yourself or a loved one, or find the right treatment path, understanding these seven critical differences is a meaningful first step toward making informed, safe choices about benzodiazepine use and recovery.