Benzodiazepine Withdrawal Timeline: What to Expect Week by Week
Understand the complete benzodiazepine withdrawal timeline week by week — symptoms, duration, risks, and how to safely manage benzo detox.
Benzodiazepine withdrawal is one of the most physically and psychologically demanding detox processes a person can go through. Unlike opioid withdrawal, which is brutal but rarely life-threatening on its own, benzo withdrawal can actually be dangerous — and in some cases, fatal — without proper medical supervision.
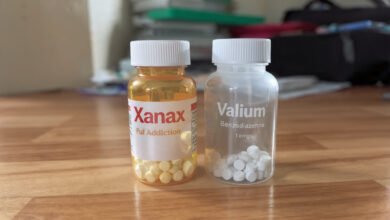
If you or someone you love is trying to stop taking benzodiazepines like Xanax (alprazolam), Valium (diazepam), Klonopin (clonazepam), or Ativan (lorazepam), understanding what lies ahead matters enormously. Knowing what to expect helps you prepare, ask the right questions, and avoid the kind of cold-turkey mistakes that send people to the emergency room.
This guide walks through the benzodiazepine withdrawal timeline week by week — what happens in your body, when symptoms typically peak, how long they last, and why some people experience symptoms that stretch on for months. We also cover the difference between short-acting and long-acting benzos, the risk of protracted withdrawal syndrome, and what the safest approaches to detox actually look like.
This is not medical advice. If you are currently taking benzodiazepines and considering stopping, please talk to a doctor before making any changes. But consider this a clear, honest guide to what the science and clinical experience actually say.
What Are Benzodiazepines and Why Is Withdrawal So Hard?
Benzodiazepines are a class of central nervous system (CNS) depressants prescribed for anxiety, panic disorder, insomnia, seizures, and muscle spasms. They work by enhancing the activity of gamma-aminobutyric acid (GABA), a neurotransmitter that slows down brain activity. When GABA binds to its receptors, it creates a calming effect — reduced anxiety, muscle relaxation, and sedation.
The problem is that with regular use, the brain adapts. It downregulates its own GABA production and upregulates excitatory neurotransmitters to compensate for the constant sedation. The brain essentially recalibrates itself around the presence of the drug. When you remove the benzo, the excitatory systems that were being suppressed suddenly have nothing holding them back. The result is a hyperexcitability state that can manifest as anxiety, insomnia, tremors, sweating, and — in severe cases — seizures.
This is also why benzodiazepine dependence can develop even when you take the medication exactly as prescribed. Physical dependence is not the same as addiction, but it does mean your brain has changed structurally, and stopping abruptly is dangerous.
Short-Acting vs. Long-Acting Benzodiazepines: Why It Changes Everything
The benzo withdrawal timeline is heavily influenced by which specific drug you were taking, largely because of half-life differences.
Short-Acting Benzodiazepines
These include drugs like:
- Alprazolam (Xanax) — half-life of 6–27 hours
- Lorazepam (Ativan) — half-life of 10–20 hours
- Triazolam (Halcion) — half-life of 1.5–5.5 hours
With short-acting benzos, the drug clears your system quickly. Withdrawal symptoms can begin within 6–12 hours of the last dose and tend to be more intense and acute because the drop in blood concentration is steep and fast.
Long-Acting Benzodiazepines
These include:
- Diazepam (Valium) — half-life of 20–100 hours
- Clonazepam (Klonopin) — half-life of 18–50 hours
- Chlordiazepoxide (Librium) — half-life of 5–30 hours
Long-acting benzos taper themselves out more gradually, which is why diazepam withdrawal tends to be less immediately severe, though it can still produce significant symptoms and protracted recovery. This is also why many clinicians use diazepam as a conversion drug when managing withdrawal from shorter-acting benzos.
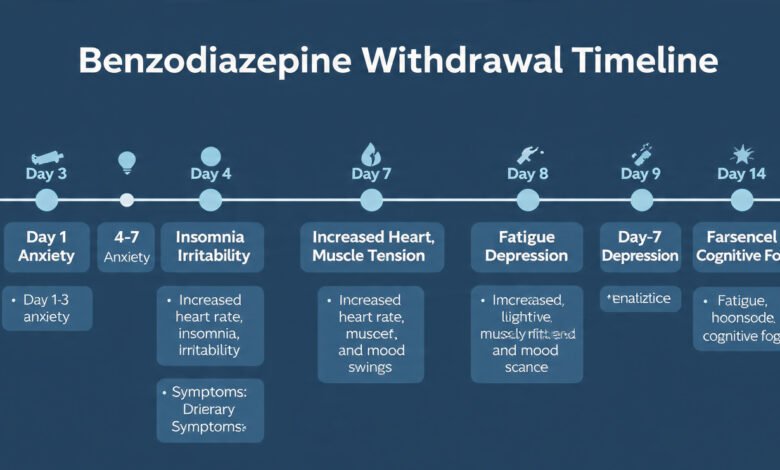
The Benzodiazepine Withdrawal Timeline: Week by Week
Phase 1: Early Withdrawal (Hours 6–96)
When symptoms start depends on which benzo you were taking.
For short-acting benzos like Xanax, the first withdrawal symptoms can appear as early as 6–12 hours after the last dose. For long-acting benzos like Valium or Klonopin, the onset is typically delayed — sometimes 24–48 hours or longer.
Early symptoms in the first 1–4 days typically include:
- Heightened anxiety and panic
- Insomnia and difficulty falling asleep
- Irritability and mood swings
- Sweating and hot flashes
- Heart palpitations
- Muscle tension and tremors
- Headache
- Rebound anxiety — anxiety that feels more severe than it did before starting the medication
One of the most important early-phase risks is seizure. Grand mal seizures can occur within the first 24–72 hours of stopping benzodiazepines abruptly, especially in people who were taking high doses or using them for extended periods. This is not common in all people, but the risk is real enough that benzo withdrawal should never be attempted cold-turkey without medical guidance. This point cannot be overstated.
Week 1: Acute Withdrawal Peaks
For most people, acute withdrawal peaks somewhere between days 3–7 for short-acting benzos, and days 5–10 for long-acting ones. This is typically the hardest part of the physical withdrawal process.
Common symptoms during week 1:
- Severe anxiety and panic attacks
- Insomnia that can last for days at a stretch
- Nausea and vomiting
- Muscle aches and cramps
- Dizziness and coordination problems
- Perceptual disturbances — visual or auditory sensitivity, hypersensitivity to light and sound
- Depersonalization (feeling detached from yourself or your surroundings)
- Cognitive impairment, brain fog, difficulty concentrating
In severe cases, some people experience delirium or psychosis during acute withdrawal. This is more likely in people with very heavy use or long-term dependence. It is a medical emergency.
Why is this happening? Your brain’s GABA system is dramatically underactive, while your glutamate (excitatory) system is running hot. Think of it like brakes failing on a car that’s simultaneously being pushed to full throttle. Until your brain recalibrates its own chemistry, you’re going to feel the consequences of that imbalance.
The seizure risk remains elevated through the first week and is highest in people who:
- Were taking high doses
- Used benzos for more than 6 months
- Have a history of previous benzo withdrawal seizures
- Are simultaneously withdrawing from alcohol
Week 2: Symptoms Begin to Stabilize
By the second week, most of the acute physical symptoms have started to ease — at least for people going through a supervised, medically assisted taper. The tremors usually improve. Sleep may still be poor, but many people get at least a few hours of rest per night.
What week 2 typically looks like:
- Physical symptoms (nausea, muscle cramps, tremors) begin to improve
- Anxiety and depression often remain elevated, sometimes intensifying
- Sleep is still disrupted but improving
- Cognitive fog begins to lift slightly
- Appetite may return
- Emotional volatility — sudden crying, anger, or low mood — is common
It is important to recognize that some of what feels like returning anxiety disorder symptoms during this window is actually rebound anxiety from the drug’s removal, not evidence that you “need” the medication to function. This is one of the most psychologically challenging aspects of benzo withdrawal — it can be very hard to tell what is you and what is the drug.
Weeks 3–4: Post-Acute Transition
For many people, weeks 3–4 represent a meaningful turning point. The sharpest edges of withdrawal have softened. The physical ordeal is largely behind them. But the psychological and neurological work is far from over.
What to expect in weeks 3–4:
- Anxiety remains significant but is more manageable
- Sleep patterns improve for most people, though it is still not back to normal
- Cognitive function begins recovering
- Mood may still cycle unpredictably
- Some people begin experiencing windows of feeling genuinely well — sometimes for the first time in years
- Cravings and urges to take the medication may appear during stressful moments
- Post-acute symptoms like brain fog and emotional blunting continue
By the end of the first month, most people who experienced a medically supervised benzodiazepine taper report that the worst is behind them. But a significant subset will continue experiencing symptoms well beyond this point.
Months 2–6: The Protracted Window
Here is where benzo withdrawal diverges significantly from what many people expect. A substantial number of long-term benzo users — particularly those who took them daily for years — go on to experience what is called Post-Acute Withdrawal Syndrome (PAWS) or protracted benzodiazepine withdrawal syndrome.
PAWS can include:
- Persistent anxiety and depression
- Ongoing insomnia
- Cognitive difficulties — memory problems, difficulty reading, trouble concentrating
- Tinnitus (ringing in the ears)
- Emotional numbness or anhedonia
- Intrusive thoughts
- Muscle twitches and aches
- Fatigue and low energy
- Perceptual disturbances — static vision, floaters, visual snow
These symptoms are not continuous or equally severe every day. Most people describe them as wave-like — periods of feeling relatively okay interrupted by sudden returns of intense symptoms. This cycling pattern is actually considered characteristic of protracted benzo withdrawal and is a useful distinguishing feature when evaluating what is happening to someone months after stopping.
The Ashton Manual, written by Dr. Heather Ashton — a British physician who spent years researching benzodiazepine dependence at Newcastle University — is one of the most widely cited resources on this topic. It describes the protracted syndrome in detail and provides taper schedules that many patients and clinicians have found useful. You can access it at benzo.org.uk, a resource maintained in her name.
Beyond 6 Months: Long-Term Recovery
For most people, significant recovery happens within 6–12 months of stopping benzodiazepines. By this point, brain neuroplasticity has had time to work — the GABA receptors that were downregulated gradually recover their sensitivity, and the brain’s inhibitory/excitatory balance is restored.
That said, some individuals — particularly those who used high doses for many years — describe symptoms lasting 18 months to 2 years or longer. The research on this is still evolving, but it is well-documented enough that clinicians who specialize in benzo withdrawal take it seriously.
Signs of long-term recovery include:
- Improved sleep quality and duration
- Return of emotional responsiveness and joy
- Sharper cognitive function
- Reduction in anxiety and panic without medication
- Better physical energy and stamina
Factors That Affect How Long Withdrawal Lasts
Not everyone has the same withdrawal experience. Several factors influence how severe and prolonged the process is:
- Duration of use: The longer you used benzos, the more the brain has adapted, and the more time it needs to recover.
- Dosage: Higher doses mean greater neurological adaptation and a harder road out.
- Type of benzo: Short-acting benzos tend to produce sharper, faster peaks; long-acting ones tend to produce more drawn-out timelines.
- Method of discontinuation: Abrupt cessation is far harder and more dangerous than a slow taper. A medically supervised gradual taper is the standard of care.
- Polydrug use: Combining benzos with alcohol, opioids, or other CNS depressants complicates withdrawal significantly.
- Individual neurochemistry: Genetic differences, baseline anxiety disorders, and previous trauma all shape the withdrawal experience.
- Age: Older individuals tend to clear drugs more slowly and may have slower neurological recovery.
- Mental health history: Pre-existing anxiety disorders, depression, or PTSD can extend and intensify the withdrawal experience.
The Safest Way to Stop: Medical Detox and Tapering
The medical consensus on how to stop benzodiazepines safely is clear: slow, supervised tapering is far safer and more tolerable than abrupt cessation.
What a Taper Looks Like
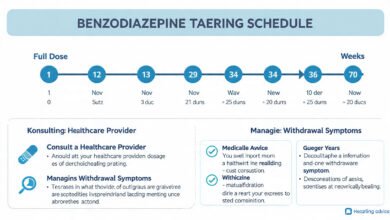
A benzodiazepine taper typically involves gradually reducing the dose over weeks or months — not days. For someone who has been on a therapeutic dose for more than a few months, a taper lasting 4–12 weeks is common. For long-term heavy users, some clinicians stretch the taper over 6 months to a year or longer.
A typical approach involves:
- Converting to an equivalent dose of a long-acting benzo (usually diazepam) if the person was taking a short-acting one
- Reducing the total daily dose by 5–10% every 1–2 weeks
- Monitoring closely for symptoms and adjusting the pace as needed
- Incorporating behavioral and psychological support alongside the physical taper
This is not a process to rush. The Ashton Manual specifically warns against decreasing more than 10% per week, and many patients need to go slower than that.
Inpatient vs. Outpatient Detox
For people with a history of seizures, high-dose use, or severe psychiatric symptoms, inpatient medical detox is typically the safest option. A supervised inpatient setting allows for continuous monitoring and immediate intervention if seizures, delirium, or other emergencies occur.
Outpatient tapering is appropriate for many people, particularly those on lower doses, with strong social support, and without a history of severe withdrawal.
The Substance Abuse and Mental Health Services Administration (SAMHSA) offers a national helpline and treatment locator to help people find appropriate care. You can reach their helpline at 1-800-662-4357 or visit findtreatment.gov to search for local treatment options.
Managing Symptoms During Withdrawal
While there is no shortcut through benzo withdrawal, several evidence-supported strategies can make the process more manageable:
Sleep Support
- Keep a consistent sleep and wake schedule
- Avoid caffeine and alcohol entirely during withdrawal
- Create a cool, dark, quiet sleep environment
- Short-term use of melatonin may help with sleep onset
Anxiety Management
- Cognitive behavioral therapy (CBT) has solid evidence for reducing anxiety without medication
- Mindfulness meditation and diaphragmatic breathing can help regulate the nervous system during acute anxiety spikes
- Regular low-to-moderate intensity exercise supports GABA recovery and mood regulation
Nutrition and Physical Recovery
- Eat regular, balanced meals — blood sugar swings worsen anxiety
- Magnesium glycinate has some evidence for supporting GABA function, though evidence is limited
- Stay hydrated
- Avoid sugar spikes and crashes
Social and Emotional Support
- Connect with peer support communities — the Benzo Buddies forum (benzobuddies.org) has helped thousands of people navigate withdrawal with community support
- Be honest with trusted family members or friends about what you are going through
- Consider working with a therapist familiar with benzo withdrawal and anxiety disorders
Common Misconceptions About Benzo Withdrawal
“If I feel better after taking more, that means I still need the medication.” This is a hallmark feature of physical dependence, not evidence that the medication is medically necessary. Relief from withdrawal symptoms when re-dosing does not validate continued use.
“I was only on a low dose, so I won’t have withdrawal.” Even low therapeutic doses taken daily for months can cause physical dependence. The dose matters, but duration matters too.
“Withdrawal should be over in a week.” For some people on short-term, low-dose use, this can be true. But for long-term users, expecting a week-long process sets up a false expectation that makes the protracted phase feel like something is wrong. Longer recovery timelines are normal and expected.
“Protracted withdrawal means I need to go back on benzos.” This is one of the most important things to resist. Going back on benzos after acute withdrawal typically restarts the dependence cycle and does not resolve the underlying neurological recovery process.
When to Seek Emergency Help
Call emergency services or go to an emergency room immediately if you or someone else experiences:
- Seizures or convulsions
- Severe confusion or disorientation (delirium)
- Hallucinations
- Extremely high fever
- Rapid or irregular heartbeat that does not settle
- Loss of consciousness
These are signs of potentially life-threatening withdrawal complications that require immediate medical attention.
Conclusion
The benzodiazepine withdrawal timeline is not a straight line. It begins within hours to days of the last dose, peaks during the first week in acute withdrawal, and then gradually improves over the following weeks and months — though a significant number of long-term users experience protracted withdrawal symptoms that can last well into the first year of recovery.
The process is shaped by which benzo you were taking, how long and at what dose, how you stopped, and your individual neurobiology. A slow, medically supervised taper is the safest and most evidence-supported approach to stopping benzodiazepines, and building in both clinical and peer support during the process gives you the best chance of getting through it successfully. Recovery is possible — the brain is remarkably capable of healing — but it takes patience, the right support, and a realistic understanding of what the journey actually looks like.