How Long Does Benzodiazepine Detox Take?
Wondering how long benzodiazepine detox takes? Discover the full benzo detox timeline, withdrawal stages, and what to expect during medically supervised treatment.

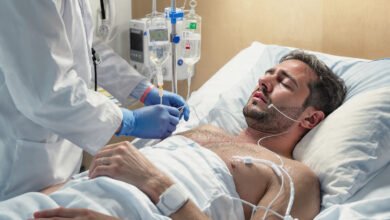
Benzodiazepine detox is one of the most medically serious withdrawal processes a person can go through. Unlike alcohol or opioids — which get most of the public attention — benzo withdrawal can be life-threatening if not handled correctly. Yet millions of people every year find themselves physically dependent on medications like Xanax, Valium, Klonopin, or Ativan, often after taking them exactly as prescribed.
If you or someone you care about is trying to stop using benzos, the first question that usually comes up is simple: how long is this going to take?
The honest answer is that it depends. The benzodiazepine detox timeline varies based on which drug you were taking, how long you used it, your dose, your age, and your overall health. Some people clear the acute withdrawal phase in a week or two. Others deal with lingering symptoms for months. And a small percentage experience what’s called post-acute withdrawal syndrome, which can stretch well beyond that.
This article walks you through the entire detox process — from the first hours after your last dose to the long road of recovery. We’ll cover the timeline, the symptoms, the medical options available to you, and why trying to quit cold turkey on your own is genuinely dangerous. By the end, you’ll have a clear, realistic picture of what benzo detox looks like and what kind of support actually helps.
What Are Benzodiazepines and Why Do They Cause Dependence?
Before diving into timelines, it helps to understand why benzodiazepine withdrawal is so intense in the first place.
Benzodiazepines are a class of prescription sedatives that work by enhancing the effect of gamma-aminobutyric acid (GABA) — the brain’s primary calming neurotransmitter. When GABA activity increases, the central nervous system slows down. That’s what makes benzos effective for treating anxiety, panic disorder, insomnia, seizures, and muscle spasms.
The problem is that the brain adapts. Over time, with regular use, your brain reduces its own natural GABA production because it’s been getting help from the drug. The GABA receptors become less sensitive. Your nervous system recalibrates itself around the presence of the medication.
When you stop taking benzos, your brain doesn’t instantly bounce back. The calming chemical is suddenly gone, but your CNS is still in a suppressed state. The result is a kind of neurological rebound — hyperexcitability — that can cause anxiety, insomnia, tremors, heart palpitations, and in serious cases, seizures.
Common benzodiazepines include:
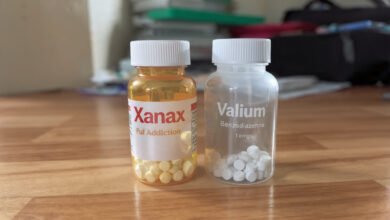
- Alprazolam (Xanax) — short-acting, high potency
- Diazepam (Valium) — long-acting, lower potency
- Lorazepam (Ativan) — intermediate-acting
- Clonazepam (Klonopin) — long-acting, used for seizures and panic
- Temazepam (Restoril) — short-acting, used for sleep
- Chlordiazepoxide (Librium) — long-acting, often used in detox protocols
The half-life of the specific benzo matters a lot when predicting the detox timeline. Short-acting benzos like Xanax leave the system quickly, so withdrawal starts sooner and often hits harder. Long-acting benzos like Valium stay in the body longer, meaning withdrawal comes on gradually but can last longer overall.
How Long Does Benzodiazepine Detox Take? The Full Timeline
The benzo detox timeline generally unfolds in three phases: early withdrawal, acute withdrawal, and post-acute withdrawal. Here’s a breakdown of each.
Phase 1: Early Withdrawal (Hours to Days)
The onset of early withdrawal depends heavily on the half-life of the benzo you were taking.
Short-acting benzos (Xanax, Ativan, Restoril): Withdrawal symptoms can begin as soon as 6 to 12 hours after the last dose. Because these drugs clear the bloodstream quickly, the brain’s calming effect disappears fast, and the rebound starts almost immediately.
Long-acting benzos (Valium, Klonopin, Librium): With these medications, early withdrawal typically begins within 24 to 48 hours after the last dose, sometimes even longer. The extended half-life means the drug is still slowly metabolizing and leaving your system over the first day or two.
Common early withdrawal symptoms include:
- Increased anxiety and irritability
- Trouble sleeping
- Restlessness
- Mild tremors
- Headaches
- Nausea or upset stomach
- Sensitivity to light and sound
At this stage, symptoms may feel like a bad flu combined with intense anxiety. Many people at this point describe feeling like their nerves are “raw.”
Phase 2: Acute Withdrawal (Days 1–14)
This is typically the most intense phase of benzodiazepine detox, and the phase that carries the most medical risk.
For short-acting benzos, peak withdrawal usually occurs around days 2 through 4. For long-acting benzos, the peak often comes between days 5 and 8.
This is the window when the most dangerous symptoms can occur, which is why medical supervision during this period is so critical.
Acute withdrawal symptoms can include:
- Severe anxiety, panic attacks
- Insomnia (sometimes total inability to sleep)
- Profuse sweating
- Heart palpitations and elevated blood pressure
- Muscle cramps and spasms
- Cognitive confusion or brain fog
- Hypersensitivity to stimuli
- Seizures — a potentially life-threatening complication
- Psychosis — rare but documented, especially in high-dose users
- Depersonalization and derealization
The seizure risk is the primary reason medical professionals strongly advise against quitting benzos cold turkey. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), benzodiazepine withdrawal is one of only two drug withdrawal syndromes — along with alcohol — that can directly cause death. A proper medical detox protocol dramatically reduces this risk.
By the end of the second week, most physically healthy people will be past the worst of the acute phase, though residual symptoms often persist.
Phase 3: Post-Acute Withdrawal Syndrome (Weeks to Months)
This is where benzo detox gets more complicated — and where a lot of people are caught off guard.
Post-acute withdrawal syndrome (PAWS) refers to a cluster of symptoms that continue after the acute phase is over. Not everyone experiences PAWS, but it’s common enough that anyone going through benzodiazepine withdrawal should understand it exists.
PAWS can last anywhere from a few weeks to 6 to 18 months, and in some cases — particularly in people who used high doses for many years — symptoms can persist even longer. The timeline is highly individual and doesn’t follow a neat schedule.
Common PAWS symptoms include:
- Persistent anxiety and depression
- Cognitive difficulties (memory problems, difficulty concentrating)
- Emotional numbness or mood swings
- Fatigue and low energy
- Insomnia or disrupted sleep patterns
- Physical symptoms like tingling, muscle aches, or GI discomfort
- Protracted cravings
The neurological healing happening during this phase is real and measurable. Brain imaging studies have shown that GABA receptor function continues to normalize for months after stopping benzos — it’s not just psychological. This is why patience and ongoing clinical support are essential.
Factors That Affect the Benzo Detox Timeline
There’s no one-size-fits-all answer to how long benzodiazepine detox takes because several variables push the timeline shorter or longer.
Type of Benzodiazepine
As discussed, the half-life is one of the biggest determining factors. Short-acting benzos move through your system faster, creating a sharper, faster withdrawal curve. Long-acting benzos produce a slower, more drawn-out process.
Dosage and Duration of Use
Someone who took a low therapeutic dose of Klonopin for 6 months will have a very different experience than someone who has been taking high-dose Xanax for 5 years. Higher doses and longer periods of use generally mean a more severe and longer-lasting withdrawal. Physical dependence can develop in as little as 2 to 4 weeks of regular use — which surprises most people.
Method of Discontinuation
Cold turkey vs. tapering is one of the most important distinctions in benzo detox.
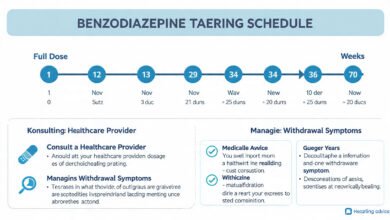
Quitting cold turkey is dangerous and is strongly discouraged by medical professionals. A gradual tapering schedule — slowly reducing the dose over weeks or months — is the standard of care because it gives the brain time to readjust. The Ashton Manual, developed by Dr. Heather Ashton and widely referenced in clinical settings, outlines tapering protocols that many physicians and addiction specialists use as a framework.
Individual Physiology
Age, liver function, mental health history, and genetics all play a role. Older adults tend to have slower drug metabolism, which can extend the timeline. People with co-occurring anxiety or depression may find withdrawal symptoms more intense since those underlying conditions re-emerge during detox.
Polydrug Use
If someone has been combining benzos with alcohol, opioids, or other substances, the detox process becomes more complicated. Both alcohol and benzos act on GABA receptors, so simultaneous withdrawal from both carries significant risk. This situation almost always requires inpatient medical management.
Benzodiazepine Detox Methods: What Actually Works
Understanding the timeline is one thing. Understanding what to do about it is another.
Medical Detox (Inpatient)
Medical detox in an inpatient or residential setting is widely considered the safest approach for benzodiazepine withdrawal, especially for people with a history of high-dose or long-term use. A medical team monitors vitals, manages complications, and can intervene immediately if seizures or severe psychological symptoms occur.
Physicians typically use one of two strategies:
- Substituting a longer-acting benzo (usually diazepam or chlordiazepoxide) for the shorter-acting benzo the person was using, then tapering the longer-acting drug slowly.
- Gradual dose reduction of the original medication, if the person was taking something that can be tapered directly.
Supportive medications may also be used to manage specific symptoms. Beta-blockers can help with elevated heart rate and blood pressure. Anticonvulsants like carbamazepine or gabapentin are sometimes used to help prevent seizures and manage neurological excitability.
Outpatient Detox
For people with mild to moderate dependence who have strong social support, outpatient detox under close physician supervision is an option. This typically involves frequent check-ins, a structured tapering schedule, and clear protocols for what to do if symptoms escalate. It’s not appropriate for everyone, and the patient and physician need to be honest about the level of risk.
The Ashton Protocol
The Ashton Manual is a comprehensive guide to withdrawing from benzodiazepines that was developed by Dr. Heather Ashton over decades of clinical work with benzo-dependent patients. It remains one of the most detailed and respected resources for both patients and clinicians. It outlines specific tapering schedules, explains the neurophysiology in plain language, and is available free online. Many patients and physicians use it as a starting point for building a personalized tapering plan.
Why Cold Turkey Benzo Detox Is Dangerous
This point deserves its own section because it’s one of the most misunderstood aspects of benzo withdrawal.
Many people assume that willpower is enough — that if you just push through the discomfort, you’ll come out the other side. With opioids, that approach is miserable but generally survivable. With benzos, it can be fatal.
When someone abruptly stops taking benzodiazepines after developing significant physical dependence, the CNS hyperexcitability that results can trigger grand mal seizures without warning. These seizures can cause brain damage, cardiac arrest, or death. The risk is real and documented, not exaggerated.
Beyond seizures, extreme delirium and acute psychosis can occur in high-dose users during abrupt discontinuation. These states are disorienting and dangerous, both for the person experiencing them and for those around them.
The bottom line: never attempt to stop benzodiazepines cold turkey after significant or prolonged use without medical guidance. If you’re unsure what counts as “significant use,” call a doctor or addiction specialist and let them make that assessment. It costs nothing to be cautious here.
Benzo Detox at Home: Is It Ever Safe?
This is a question a lot of people ask, and it deserves an honest answer.
For people with very low-level, short-term benzodiazepine use — say, someone who took a therapeutic dose for 3 to 4 weeks and wants to stop — gradual self-tapering under a doctor’s guidance may be feasible. But that’s a narrow category.
For the vast majority of people asking this question — those who have been using benzos for months or years, at higher doses, or who have experienced withdrawal symptoms before — home detox is high-risk. Without the ability to monitor vital signs, respond to a seizure, or intervene in a psychiatric emergency, the consequences of something going wrong are severe.
If cost or access is the barrier, contact SAMHSA’s National Helpline at 1-800-662-4357 — it’s free, confidential, and available 24/7. They can connect you with low-cost or no-cost treatment options in your area.
What to Expect After Benzo Detox: Recovery and Beyond
Getting through benzodiazepine detox is a significant accomplishment, but it’s the beginning of recovery, not the end.
Managing PAWS
The lingering symptoms of post-acute withdrawal can be discouraging, especially when they show up weeks or months after you thought you were done. It helps to know that this is a normal part of the neurological healing process and that it does get better.
Practical strategies for managing PAWS include:
- Regular sleep schedule — disrupted sleep is one of the most persistent PAWS symptoms, and good sleep hygiene makes a measurable difference
- Physical exercise — exercise increases GABA activity naturally and helps regulate mood
- Therapy — cognitive behavioral therapy (CBT) and other evidence-based approaches help address the anxiety and thought patterns that often underlie benzo dependence
- Avoiding alcohol and other CNS depressants — these can trigger setbacks and interfere with neurological healing
- Support groups — organizations like Benzo Buddies (an online peer support community) provide connection with others who understand the specific challenges of benzo withdrawal
Addressing the Underlying Reasons
Most people who develop problematic benzo use were originally prescribed the medication for a legitimate reason — usually anxiety, panic disorder, or insomnia. After detox, those underlying conditions still need to be addressed, ideally with non-habit-forming treatments.
Options include:
- SSRIs or SNRIs for long-term anxiety and depression management
- CBT for anxiety disorders and insomnia (CBT-I is particularly effective for sleep)
- Mindfulness-based stress reduction (MBSR)
- Buspirone for generalized anxiety disorder
- Hydroxyzine for situational anxiety
Working with a psychiatrist who understands benzo dependence and recovery is invaluable here.
Special Considerations: Who Is at Highest Risk?
Certain populations face a higher risk of severe complications during benzodiazepine detox and need extra caution.
Long-Term, High-Dose Users
People who have been taking benzos daily for years, especially at higher-than-prescribed doses, have a deeply recalibrated nervous system. Their detox timeline will be longer, their symptoms potentially more severe, and their PAWS phase potentially more prolonged.
Older Adults
Elderly patients metabolize drugs more slowly and are more sensitive to neurological disruptions. Seizure risk, falls, and cognitive complications during withdrawal are all elevated in this group.
People with Co-Occurring Mental Health Conditions
Anxiety disorders, depression, PTSD, and bipolar disorder are all common in people who develop benzo dependence. These conditions can intensify withdrawal symptoms and increase the risk of relapse after detox. Integrated treatment — addressing both the substance dependence and the mental health condition simultaneously — produces significantly better outcomes.
People with a History of Seizures
Prior seizure history, from any cause, increases the risk of withdrawal-related seizures. These individuals should almost always detox in an inpatient medical setting with anticonvulsant coverage.
How Long Does Benzo Detox Take? A Summary by Drug Type
Here’s a quick reference overview of the benzodiazepine detox timeline by medication:
| Benzodiazepine | Half-Life | Withdrawal Onset | Peak Symptoms | Acute Phase Duration |
|---|---|---|---|---|
| Alprazolam (Xanax) | 6–27 hours | 6–12 hours | Days 2–4 | 5–14 days |
| Lorazepam (Ativan) | 10–20 hours | 12–24 hours | Days 3–5 | 7–14 days |
| Clonazepam (Klonopin) | 18–50 hours | 24–48 hours | Days 5–7 | 10–21 days |
| Diazepam (Valium) | 20–100 hours | 48–72 hours | Days 6–8 | 2–4 weeks |
| Temazepam (Restoril) | 8–20 hours | 12–24 hours | Days 2–4 | 5–14 days |
Note: These are general ranges. Individual experience can vary significantly from these averages.
Getting Help: What to Look for in a Benzo Detox Program
If you’re ready to address benzo dependence, finding the right level of care matters.
When evaluating treatment options, look for:
- Medical detox with 24/7 supervision for moderate to severe dependence
- Licensed addiction medicine physicians or psychiatrists on staff
- Individualized tapering protocols rather than one-size-fits-all approaches
- Dual diagnosis treatment if you have co-occurring mental health issues
- Continuity of care — what happens after detox? Is there a transition to residential, outpatient, or ongoing therapy?
Don’t hesitate to ask questions before committing to a program. A reputable facility will be transparent about their protocols, staff credentials, and success metrics.
Conclusion
Benzodiazepine detox is a serious, multi-phase process that can take anywhere from a couple of weeks to well over a year depending on the person, the drug, the dose, and the duration of use. The acute withdrawal phase for most benzos runs roughly one to three weeks, but post-acute withdrawal syndrome can extend the recovery timeline significantly.
The most critical thing to understand is that benzo withdrawal is medically dangerous — particularly the risk of seizures during abrupt discontinuation — and that attempting to quit cold turkey without professional support is a genuine health risk, not just an uncomfortable inconvenience. A medically supervised detox with a structured tapering protocol is the safest and most effective path, and the support of qualified professionals, evidence-based therapies, and a solid aftercare plan dramatically improves the odds of long-term recovery.