The Hidden Epidemic: Prescription Benzodiazepine Addiction in America
Prescription benzodiazepine addiction is silently affecting millions of Americans. Discover the warning signs, withdrawal dangers, and proven recovery options.

Prescription benzodiazepine addiction doesn’t look like what most people picture when they think of drug addiction. There’s no back-alley dealer, no dramatic intervention scene. Instead, it often starts with a doctor’s appointment, a legitimate diagnosis of anxiety or insomnia, and a prescription for something that actually works — at least at first.
Benzodiazepines like Xanax, Valium, Klonopin, and Ativan are among the most prescribed medications in the United States. They calm the nervous system, ease panic attacks, and help people sleep. Millions of Americans take them exactly as directed. And yet, a growing body of evidence shows that even patients following their doctor’s orders can quietly develop a physical dependence that is remarkably difficult to escape.
According to a nationally representative study, 30.6 million American adults — about 12.6% of the population — reported past-year benzodiazepine use, with 5.3 million of those engaging in some form of misuse. The 2024 National Survey on Drug Use and Health found that 4.6 million Americans misused prescription tranquilizers or sedatives in the past year alone.
This is not a fringe problem. It is a full-scale public health crisis hiding in plain sight — inside medicine cabinets, nursing homes, and primary care waiting rooms across the country. This article breaks down how it happens, who it affects, and what can actually be done about it.
What Are Benzodiazepines?
Benzodiazepines (commonly called “benzos”) are a class of central nervous system (CNS) depressants that work by enhancing the effect of gamma-aminobutyric acid, or GABA — the brain’s primary inhibitory neurotransmitter. When GABA activity increases, neural communication slows down, producing feelings of calm, sedation, muscle relaxation, and relief from anxiety.
They were first developed in the 1950s and became wildly popular by the 1970s as a safer alternative to barbiturates. For decades, they were considered a medical success story. The problem is that the medical community significantly underestimated just how habit-forming they are, and how quickly the brain adapts to their presence in ways that make stopping genuinely dangerous.
Common Benzodiazepines Prescribed in America
The benzo family includes dozens of compounds, but a handful dominate U.S. prescriptions:
- Alprazolam (Xanax) — prescribed primarily for anxiety and panic disorder
- Diazepam (Valium) — used for anxiety, muscle spasms, and alcohol withdrawal
- Clonazepam (Klonopin) — prescribed for panic disorder and seizures
- Lorazepam (Ativan) — commonly used for anxiety and as a pre-surgical sedative
- Temazepam (Restoril) — prescribed mainly for short-term insomnia
- Oxazepam (Serax) — used for anxiety and alcohol withdrawal symptoms
In 2024, U.S. pharmacies dispensed 30.5 million prescriptions for alprazolam (Xanax), 21.4 million for clonazepam (Klonopin), 19.8 million for lorazepam (Ativan), and 8.2 million for diazepam (Valium), according to the Department of Justice. Those numbers represent an enormous volume of a drug that carries significant dependency risk.
The Scale of Prescription Benzodiazepine Addiction in America
The numbers are hard to absorb, but they matter. Prescription benzodiazepine addiction and dependence in America operate at a scale that most people — including many healthcare providers — don’t fully appreciate.
From 1996 through 2013, the number of benzo prescriptions grew from 8.1 million to 13.5 million per year, a 67% rate of growth, while the number of people dying from benzo overdose increased over sevenfold during the same period.
Benzodiazepine overdose deaths climbed from 1,135 in 1999 to a peak of 11,537 in 2017, then fell modestly before rising again to 12,499 in 2021, and settling at 10,964 in 2022. Even at the lower end of that range, nearly 11,000 deaths a year is an extraordinary toll for a class of drugs that most people associate with treating anxiety rather than causing death.
Overall, 9.1% of American adults — more than 21 million people — reported benzodiazepine use in 2023.
Despite growing awareness, the epidemic continues because it is deeply embedded in how American medicine treats anxiety disorders, insomnia, and chronic stress — three of the most commonly reported conditions in the country.
How Prescription Benzodiazepine Addiction Develops
One of the most important and least-discussed truths about benzo dependence is that it can develop without any intentional misuse. You don’t have to be chasing a high, taking someone else’s pills, or doubling your dose. The brain changes on its own timeline.
The Role of GABA Receptors
When you take a benzodiazepine regularly, your brain notices the consistent increase in GABA activity and adjusts by reducing its own natural production of GABA and downregulating (reducing) GABA receptor sensitivity. This is called neuroadaptation — the brain doing exactly what it’s designed to do, which is maintain equilibrium.
The result is that after weeks or months of use, the calming effect of the drug diminishes (this is called tolerance), and your nervous system now requires the medication just to function at a baseline level. When the drug is not present, the GABA system is underactive and the brain’s excitatory systems run unopposed — producing anxiety, insomnia, tremors, and in severe cases, life-threatening seizures.
When Prescribed Use Becomes Dependence
The transition from therapeutic use to physical dependence can happen in as little as two to four weeks of daily use, according to many pharmacology experts. Most prescribing guidelines actually recommend that benzodiazepines be used for no longer than two to four weeks for this exact reason. In practice, many patients remain on them far longer.
The proportion of benzodiazepine use classified as long-term increased significantly with age, from 14.7% among adults aged 18 to 35, up to 31.4% among those aged 65 to 80. When that many people are using these medications for extended periods, physical dependence becomes almost inevitable for a significant portion of them — even at therapeutic doses prescribed by a physician.
The clinical distinction matters here: physical dependence is not the same as addiction. Dependence means your body has adapted and will go through withdrawal if the drug stops. Benzo addiction — formally called benzodiazepine use disorder — involves compulsive drug-seeking behavior, loss of control, and continued use despite harm. Both are serious. Both require medical attention. And both frequently develop when patients are simply trying to manage a legitimate health condition.
Who Is Most at Risk?
Prescription benzodiazepine addiction does not affect everyone equally. Understanding the risk factors helps both patients and clinicians make better decisions.
Women face disproportionate exposure. Benzodiazepines are more frequently prescribed to women than men, largely due to higher rates of anxiety disorders, and women are twice as likely to use benzodiazepines compared to men, with stronger cravings increasing the risk of misuse.
Older adults face some of the most serious risks. About 10% of older adults have benzodiazepine prescriptions, and an estimated 25% to 30% of those have been taking them longer than recommended — between 1.4 and 1.7 million people. This is concerning because benzos are associated with falls, cognitive decline, and delirium in elderly patients.
Young adults aged 18 to 25 show the highest rates of misuse. Those aged 18 to 25 had the highest misuse rate at 5.2%, while adults over 65 had the lowest at 0.6%.
People with co-occurring disorders face compounded risk. Misuse and abuse of or dependence on prescription opioids or stimulants were strongly associated with benzodiazepine misuse. When someone is already managing one substance dependency, the risk of developing another increases significantly.
Lower-income patients also face structural risk. Lower- and middle-income patients are more likely to become long-term users than those in higher-income areas, possibly because they have less access to alternative treatments like therapy, which can reduce reliance on medication.
The 7 Dangerous Truths About Prescription Benzodiazepine Addiction
Here are the realities that don’t make it into most conversations between doctors and patients:
- Dependence can develop even at prescribed doses. You don’t have to misuse your medication for your body to become dependent. Regular daily use at therapeutic doses over several weeks is often enough.
- Tolerance builds faster than most patients expect. What worked for your anxiety at week two may feel like it’s barely doing anything at month three. This leads many patients to gradually increase their dose, sometimes without telling their doctor.
- Stopping suddenly can kill you. Unlike opioid withdrawal, which is brutal but rarely directly fatal, benzo withdrawal can cause life-threatening seizures. This makes it one of only two drug withdrawal syndromes (along with alcohol) that can be directly fatal.
- Doctors often don’t have a clear exit plan. Many patients are placed on benzodiazepines without a defined treatment endpoint, then find themselves trapped on a medication that their doctor is reluctant to taper and unable to easily discontinue.
- The combination with opioids is deadly. Each day in the United States, 115 people die from opioid overdoses, and over 30% of those overdoses also involve benzodiazepines. The two drug classes together amplify respiratory depression in a way that can stop breathing entirely.
- Long-term use causes cognitive damage. Chronic benzodiazepine use is linked to memory impairment, reduced processing speed, and other cognitive deficits — some of which may persist even after the drug is stopped.
- Recovery from benzo dependence takes longer than most people expect. Many former users report a post-acute withdrawal syndrome (PAWS) that can last months to years after stopping, involving anxiety, insomnia, and hypersensitivity to stimuli. This prolonged suffering causes many people to relapse — not to get high, but simply to feel normal.
Benzodiazepine Withdrawal: One of the Most Dangerous in Medicine
Benzo withdrawal is not just uncomfortable — it is medically serious in a way that is still poorly understood by the general public and, in some cases, by clinicians who don’t specialize in addiction.
Withdrawal Symptoms
Symptoms of benzodiazepine withdrawal vary in intensity depending on the dose, duration of use, and the specific drug (shorter-acting benzos like Xanax produce more intense, faster-onset withdrawal than longer-acting ones like Valium). Common symptoms include:
- Severe anxiety and panic attacks (often worse than what the drug was prescribed for)
- Insomnia and sleep disturbances
- Tremors and muscle spasms
- Sweating, heart palpitations, and elevated blood pressure
- Nausea, vomiting, and diarrhea
- Cognitive impairment, confusion, and difficulty concentrating
- Depersonalization and derealization
- Seizures (in severe cases, potentially fatal)
- Psychosis (rare but documented in acute high-dose withdrawal)
Why Quitting Cold Turkey Can Be Deadly
The GABA system suppression that develops during long-term benzo use leaves the nervous system in a hyperexcitable state. Remove the drug suddenly, and that excitability has nothing to counteract it. This is the same neurological mechanism that makes alcohol withdrawal deadly, and the two syndromes are treated similarly — often with longer-acting benzodiazepines or phenobarbital in a controlled medical setting.
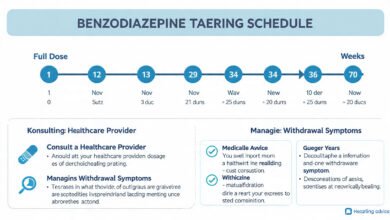
According to medical guidance, benzodiazepines “should not be discontinued abruptly if patients have been taking them for more than a month; they must be tapered gradually with guidance from a provider.”
The Ashton Manual, developed by British pharmacologist Professor Heather Ashton over years of working with benzo-dependent patients, remains one of the most referenced resources for benzodiazepine tapering protocols worldwide, even though it is not an officially endorsed medical guideline. The Benzodiazepine Information Coalition has compiled substantial research on long-term outcomes and withdrawal protocols that patients and clinicians can access freely.
The Hidden Connection Between Benzos and the Opioid Crisis
The opioid epidemic has dominated headlines for years, and rightly so. But what often goes unmentioned is how deeply prescription benzodiazepine addiction is intertwined with opioid deaths.
In 2019, benzodiazepines were a factor in 16% of all opioid-related overdose deaths. In 2021, nearly 14% of all opioid-caused overdose deaths also involved benzodiazepines.
Both drug classes slow breathing. Together, their effect on the respiratory system is synergistic — meaning the combination is far more dangerous than either drug alone. A person who has built tolerance to both substances may not realize they have crossed into lethal territory until it is too late.
The rate of co-prescribing benzodiazepines with opioids quadrupled from 0.5% in 2003 to 2% in 2015. That’s a fourfold increase in a practice that every major medical organization has warned against — happening right inside the mainstream healthcare system.
In 2022, among drug-related emergency department visits that involved multiple substances, 73% involved benzodiazepines. That single statistic speaks to how often benzos are at the scene of a drug emergency, even when they are not the primary drug of concern.
Why Doctors Keep Prescribing Them
It would be easy to cast this as a story of reckless medicine, but the reality is more complicated. Benzodiazepines work. For generalized anxiety disorder, panic disorder, alcohol withdrawal, and certain seizure conditions, they are highly effective in the short term. Nothing in medicine is a clean trade-off.
The percentage of outpatient medical visits that led to a benzodiazepine prescription doubled — from 3.8% to 7.4% — between 2003 and 2015, with the prescribing rate among primary care doctors more than doubling, from 3.6% to 7.5% of visits.
Primary care physicians, not psychiatrists, are now the primary source of most benzodiazepine prescriptions in the United States. These are doctors who are also managing diabetes, heart disease, cancer screenings, and dozens of other conditions during 15-minute appointments. They are not always equipped to monitor for the early signs of benzo dependence, follow complex tapering protocols, or provide the psychotherapy-based alternatives that would reduce reliance on the medication.
There is also the reality of patient demand. Anxiety is genuinely debilitating. When someone walks into a clinic in the grip of a panic disorder, offering them twelve weeks of cognitive behavioral therapy and telling them to come back if it doesn’t work is not always a realistic option. The pill solves the immediate problem.
As one psychiatrist put it, “It’s a shift in the philosophy of how to treat anxiety.” That shift is happening, but slowly, and a great deal of human suffering is accumulating in the gap.
Treatment Options for Prescription Benzodiazepine Addiction
The good news is that prescription benzodiazepine addiction is treatable, and people do fully recover — though it takes time and the right kind of support. There is no single correct path, but several approaches have solid evidence behind them.
Medical Detox and Supervised Tapering
For most people with benzo dependence, the first step is a medically supervised taper — gradually reducing the dose over weeks to months to allow the brain to readjust. This is not the same as detox from opioids or stimulants; it requires careful planning and consistent monitoring.
Common approaches include:
- Direct tapering — slowly reducing the patient’s current benzo dose at a rate they can tolerate, often no faster than 5-10% every 1-4 weeks
- Substitution tapering — switching to a longer-acting benzodiazepine (usually diazepam/Valium) to smooth out the pharmacological curve, then tapering that drug gradually
- Inpatient medical detox — for high-dose or complex cases, particularly those with a history of seizures or polysubstance use
The Substance Abuse and Mental Health Services Administration (SAMHSA) provides treatment locator tools and clinical guidance for both patients and providers navigating benzo withdrawal and recovery.
Behavioral Therapy and Long-Term Recovery
Medication management gets someone off the drug. Therapy addresses why they needed it in the first place and builds the tools to stay off it.
Evidence-based therapies for benzodiazepine use disorder and the underlying conditions it treats include:
- Cognitive Behavioral Therapy (CBT) — the most well-researched treatment for anxiety disorders, and highly effective for reducing reliance on medication
- Mindfulness-Based Stress Reduction (MBSR) — teaches patients to tolerate anxiety and discomfort without pharmacological help
- Motivational Interviewing (MI) — helps patients clarify their goals and build intrinsic motivation to change
- Group therapy and peer support — particularly important for people who feel isolated by a dependency that others may not understand or take seriously
For many patients, the combination of a slow medical taper and concurrent psychotherapy produces the best long-term outcomes. Recovery from benzo addiction is not simply about eliminating a chemical — it requires rebuilding a nervous system that has been rewired by years of pharmacological dependence.
Alternatives to Benzodiazepines for Anxiety and Insomnia
One of the reasons prescription benzodiazepine addiction persists is that many patients and doctors don’t know what else to reach for. Here are some alternatives with a reasonable evidence base:
For anxiety and panic disorder:
- SSRIs and SNRIs (antidepressants like sertraline, escitalopram, venlafaxine) — first-line treatments for most anxiety disorders, non-addictive, and effective for long-term management
- Buspirone — an anti-anxiety medication with no addiction potential, though it takes 2-4 weeks to work
- Beta-blockers (like propranolol) — can address the physical symptoms of anxiety and panic in certain situations
- CBT and exposure therapy — arguably the most durable treatment available for anxiety disorders
For insomnia:
- CBT for Insomnia (CBT-I) — the gold-standard first-line treatment for chronic insomnia, consistently outperforming sleep medication in long-term outcomes
- Sleep hygiene protocols — not glamorous, but genuinely effective for many people
- Melatonin — limited evidence but very low risk, appropriate for circadian rhythm-related sleep issues
- Low-dose doxepin — FDA-approved for insomnia, not habit-forming
None of these alternatives are as immediately powerful as a benzodiazepine at calming an acute anxiety attack or producing sleep on demand. That gap in immediate effectiveness is real. But for the millions of people caught in long-term benzo dependence, the short-term power of the drug was the source of the problem, not the solution.
Conclusion
Prescription benzodiazepine addiction represents one of America’s most underacknowledged public health crises — a problem hiding inside the healthcare system itself, affecting tens of millions of people who sought treatment for anxiety, insomnia, or stress and ended up dependent on a drug that is genuinely difficult to stop. The data is unambiguous: benzodiazepines carry serious risks for physical dependence, cognitive impairment, and fatal overdose, particularly when combined with opioids, and yet they continue to be prescribed at enormous scale with insufficient attention to exit strategies or patient monitoring.
The path forward requires better prescribing practices, broader access to therapy-based alternatives, improved medical training on benzo withdrawal and tapering protocols, and — most importantly — honesty with patients about what these drugs actually do to the brain over time. People living with benzodiazepine dependence deserve the same urgency and compassion that we extend to those struggling with any other chronic disease.