How to Quit Benzodiazepines Safely: A Step-by-Step Guide
Learn how to quit benzodiazepines safely with this step-by-step guide covering tapering schedules, withdrawal symptoms, and expert-backed recovery strategies.

How to quit benzodiazepines safely is one of the most searched — and most misunderstood — questions in modern healthcare. Every year, millions of people who were prescribed these medications for anxiety, insomnia, or seizure disorders find themselves physically dependent, often without fully realizing how it happened. Benzodiazepines like Xanax (alprazolam), Valium (diazepam), Ativan (lorazepam), and Klonopin (clonazepam) are genuinely effective drugs for short-term use. The problem is that the brain adapts to them quickly — sometimes within just two to four weeks of regular use.
Once dependence takes hold, stopping suddenly is not just uncomfortable. It can be dangerous. Benzodiazepine withdrawal is one of the few drug withdrawal syndromes that can actually kill you, putting it in the same category as alcohol withdrawal. Seizures, psychosis, and life-threatening cardiovascular instability are real risks for people who stop cold turkey.
The good news is that with the right plan, the right support, and a medically supervised benzo taper, most people can discontinue benzodiazepines successfully. This guide walks you through exactly what that process looks like — step by step, without sugarcoating the challenges or the timeline involved.
What Are Benzodiazepines and Why Are They So Hard to Quit?
Benzodiazepines are a class of central nervous system (CNS) depressants that work by amplifying the effects of gamma-aminobutyric acid (GABA) — the brain’s primary calming neurotransmitter. When you take a benzo, GABA activity increases, nerve signals slow down, and you feel relaxed, sedated, or less anxious.
The catch is that your brain notices this extra GABA activity and compensates. Over time, it downregulates its own GABA receptors, meaning it produces less natural calming activity on its own. When the medication is removed, the brain can’t restore balance quickly. The result is a nervous system that becomes hyperexcited — producing anxiety, tremors, insomnia, and in severe cases, seizures.
Common benzodiazepines and their approximate half-lives:
- Alprazolam (Xanax) — 6–27 hours (short-acting)
- Lorazepam (Ativan) — 10–20 hours (short-acting)
- Clonazepam (Klonopin) — 18–50 hours (intermediate)
- Diazepam (Valium) — 20–100 hours (long-acting)
- Chlordiazepoxide (Librium) — 24–100 hours (long-acting)
Short-acting benzodiazepines tend to produce more intense, faster-onset withdrawal symptoms. Long-acting ones clear more slowly, creating a more gradual but prolonged withdrawal experience.
Physical dependence can develop in as little as two to four weeks of daily use at therapeutic doses. This is not the same as addiction — many people who become dependent on benzodiazepines never misuse them, never take more than prescribed, and are genuinely surprised when they struggle to stop.
Step 1: Talk to Your Doctor Before You Do Anything Else
The single most important thing you can do is tell your prescribing doctor that you want to discontinue your benzodiazepine. This is not a conversation to put off or avoid.
Many people hesitate because they feel embarrassed about their dependence or worry their doctor will judge them. But most physicians are well aware that long-term benzodiazepine use creates physical dependence in a significant percentage of patients. A good doctor will not blame you — they will help you build a safe exit plan.
During this conversation, your doctor will want to know:
- Which benzodiazepine you’re taking and the current dose
- How long you’ve been taking it
- Whether you use any other substances (including alcohol)
- Your general health status and any other medications
- Your history of seizures or anxiety disorders
Based on this, they will help you decide whether to taper directly from your current benzo, or whether switching to a longer-acting benzodiazepine like diazepam first makes more sense for your situation.
If your doctor is dismissive or unwilling to help, seek a second opinion. A psychiatrist, addiction medicine specialist, or internist familiar with benzodiazepine deprescribing can all help. You deserve a partner in this process.
Step 2: Understand the Difference Between Tapering Methods
There are two primary approaches to benzodiazepine tapering, and understanding both helps you have a more informed conversation with your provider.
Direct Taper
A direct taper means gradually reducing the dose of the benzodiazepine you’re already taking. This is often the preferred approach when:
- You’re already on a long-acting benzo
- Your current dose is relatively low
- You’ve been taking it for less than a year
- Withdrawal symptoms during previous attempts were manageable
The standard rate recommended by most clinical guidelines is a 10–25% dose reduction every one to two weeks, though slower reductions are common and appropriate. Some protocols favor a 5–10% reduction per month for people who have been on higher doses for many years.
Substitution Taper (Diazepam Switch)
A substitution taper involves converting your current benzodiazepine to an equivalent dose of diazepam (Valium) before beginning the taper. Diazepam is favored for this purpose because:
- It has a very long half-life (20–100 hours) and produces a smoother, more stable blood level
- It’s available in multiple dose sizes and can be taken in liquid form for fine-grained reductions
- The gradual clearance reduces the “peaks and valleys” that cause breakthrough withdrawal symptoms
This approach is detailed in the widely referenced Ashton Manual — a comprehensive guide to benzodiazepine tapering written by Professor Heather Ashton, a British pharmacologist who ran one of the first dedicated benzo withdrawal clinics. While some newer clinical guidelines have updated certain Ashton recommendations — particularly around the speed of tapering — the foundational principles remain valuable and widely cited.
Step 3: Build a Realistic Tapering Schedule
One of the biggest reasons benzo tapers fail is that people (and sometimes their doctors) set an overly aggressive timeline. The clinical evidence is clear: slower tapers produce better outcomes and fewer complications.
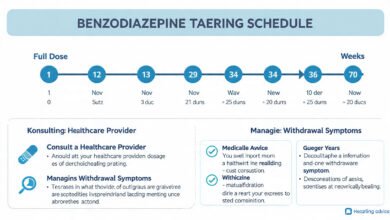
A realistic schedule might look like this:
For someone taking 2mg lorazepam daily for 3 years:
| Week | Daily Dose |
|---|---|
| 1–2 | 1.75 mg |
| 3–4 | 1.5 mg |
| 5–6 | 1.25 mg |
| 7–8 | 1.0 mg |
| 9–10 | 0.75 mg |
| 11–12 | 0.5 mg |
| 13–14 | 0.25 mg |
| 15–16 | Discontinue |
In practice, most people need to pause or slow down at some points during the taper — and that is completely normal. The schedule is a guide, not a contract.
Factors that typically require a slower taper:
- Long duration of use (3+ years)
- High doses at the start
- Previous failed withdrawal attempts
- Concurrent use of other CNS-depressant medications
- History of anxiety disorders, PTSD, or seizures
- Older age
What to do if breakthrough symptoms hit:
- Hold the current dose and don’t reduce further until symptoms stabilize
- Discuss with your doctor whether a temporary dose increase is appropriate
- Rule out other causes (illness, stress, sleep deprivation)
- Never skip doses or make unsupervised changes to the schedule
Step 4: Know What to Expect — Benzodiazepine Withdrawal Symptoms
Understanding benzo withdrawal symptoms before they happen takes some of the fear out of the process. These symptoms are real, and they can be intense, but they are also temporary.
Short-Acting Benzo Withdrawal Timeline
For drugs like Xanax and Ativan, acute withdrawal symptoms typically begin within 6–24 hours of the last dose and peak around days 2–4. Most physical symptoms improve within 5–7 days.
Long-Acting Benzo Withdrawal Timeline
For drugs like Valium and Klonopin, symptoms may not begin until 1–2 days after the last dose and can persist for 2–4 weeks. The prolonged half-life means a more gradual but extended experience.
Common Withdrawal Symptoms
Mild to moderate:
- Anxiety and irritability
- Insomnia and disturbed sleep
- Muscle tension and aches
- Headaches
- Sweating and hot flashes
- Difficulty concentrating
Moderate to severe:
- Tremors and shakiness
- Heart palpitations
- Nausea and vomiting
- Heightened sensory sensitivity (light, sound, touch)
- Panic attacks
- Depersonalization or derealization
Severe (requires immediate medical attention):
- Seizures
- Psychosis or hallucinations
- Severe confusion
- High fever
- Suicidal thoughts
What Is Rebound Anxiety?
Rebound anxiety is a return of the symptoms the medication was originally treating — typically more intensely than before. It’s one of the most disorienting parts of benzo withdrawal because it can feel like evidence that you “need” the medication. In most cases, rebound anxiety is temporary and peaks in the first one to two weeks before gradually subsiding as the nervous system rebalances.
Protracted Withdrawal Syndrome (PAWS)
A meaningful percentage of long-term users experience protracted withdrawal syndrome — a condition where a subset of symptoms (most commonly anxiety, insomnia, and cognitive fog) persist for weeks, months, or in rare cases longer after the medication is stopped. The symptoms tend to come in waves rather than being constant, and they do improve over time. Patience and continued support are critical.
Step 5: Manage Withdrawal Symptoms Without Jumping Back to Benzos
There are several evidence-based strategies for managing benzodiazepine withdrawal symptoms that don’t involve returning to the medication. Think of these as tools in your toolkit:
Non-Medication Approaches
Sleep hygiene: Insomnia is one of the most common and distressing withdrawal symptoms. Strict sleep hygiene practices — consistent wake times, dark and cool sleeping environment, no screens before bed, limiting caffeine after noon — can meaningfully improve sleep quality without medication.
Exercise: Regular aerobic exercise has been shown to reduce anxiety and improve sleep. Even 30 minutes of walking daily can make a difference, and it naturally increases GABA activity.
Mindfulness and breathing exercises: Cognitive behavioral therapy (CBT) and mindfulness-based stress reduction (MBSR) have solid evidence for reducing anxiety. Learning to observe anxious thoughts without reacting to them is a skill that becomes increasingly valuable as you taper.
Nutrition and hydration: Staying well hydrated, maintaining stable blood sugar, and reducing alcohol and caffeine can ease symptom intensity.
Medical Symptom Management
Your doctor may consider the following adjunct medications in specific situations:
- Anticonvulsants (like gabapentin or carbamazepine) may reduce withdrawal severity and seizure risk
- Beta-blockers (like propranolol) can help with palpitations and physical anxiety symptoms
- Melatonin or sedating antihistamines may assist with sleep in early withdrawal
- Antidepressants may be appropriate if underlying depression or anxiety disorder is present
What doctors will typically avoid are other habit-forming sedatives, which carry their own dependence risks. The goal is to get your nervous system back to functioning without chemical props, not to replace one dependency with another.
Step 6: Build Your Support System
Quitting benzodiazepines is not something most people should try to do alone — not just for medical safety reasons, but for emotional ones. The withdrawal process can last months, and there will be hard days. Having the right support structure dramatically improves the odds of success.
Medical support: Make sure you have a doctor or prescriber who knows your taper schedule and is reachable if things go wrong. Regular check-ins — even brief phone calls — can catch problems early.
Mental health support: A therapist familiar with benzodiazepine dependence can be invaluable. CBT in particular has strong evidence for both anxiety disorders and substance use. Therapy helps you address whatever originally drove the prescription, which reduces the risk of relapse after discontinuation.
Peer support: There is a growing community of people who have been through benzo withdrawal. Online forums and support groups — such as those organized around The Benzodiazepine Information Coalition — offer practical advice and genuine empathy from people who understand what the process actually feels like.
Family and friends: The people closest to you don’t need to fully understand benzodiazepine pharmacology. They just need to know that you’re going through something real and that consistent, non-judgmental support matters. Be honest with at least one trusted person about what you’re doing.
Step 7: Plan for Life After Benzodiazepines
The final phase of quitting benzodiazepines safely is what comes after the taper is complete. This is sometimes under-discussed, but it matters enormously.
Address the Underlying Condition
Benzodiazepines were usually prescribed for a reason — anxiety, panic disorder, PTSD, insomnia, or something else. Stopping the medication doesn’t make that reason disappear. The months leading up to and following discontinuation are a good time to actively build non-pharmaceutical approaches:
- CBT for anxiety is highly effective and produces durable results
- Acceptance and Commitment Therapy (ACT) is particularly useful for people dealing with health anxiety
- EMDR (Eye Movement Desensitization and Reprocessing) is evidence-based for trauma and PTSD
- Lifestyle factors — sleep, exercise, diet, stress management — are not adjuncts; they’re central
Relapse Prevention
It’s worth having an honest conversation with yourself (and your doctor) about scenarios that might make you want to restart benzos. Knowing your triggers in advance — major life stress, insomnia flares, anniversary reactions — lets you plan alternative responses rather than reaching for a prescription.
If you do relapse, that’s not a catastrophe. Report it to your doctor, don’t increase the dose or frequency, and resume your tapering plan. Relapse is a normal part of many people’s discontinuation journey, not a sign that you’ve failed.
According to the American Society of Addiction Medicine, combining behavioral therapy with a medically supervised taper produces significantly better long-term outcomes than tapering alone. ASAM’s 2025 Benzodiazepine Tapering Guidelines are a useful reference for both patients and providers navigating this process.
How to Quit Benzodiazepines Safely: Special Situations
Pregnant Women
Benzodiazepine withdrawal during pregnancy requires specialist input. Both the risks of withdrawal and the risks of continued use must be carefully weighed. Abrupt discontinuation is generally considered more dangerous than a supervised taper, but the rate and approach need to be guided by both an obstetrician and a maternal-fetal medicine specialist.
Older Adults
Older adults are more vulnerable to the cognitive side effects of benzos and also to the complications of withdrawal, including a heightened seizure risk. Slower tapers and close monitoring are especially important in this population.
People Using High Doses or Multiple Benzos
If you’ve been using doses significantly above the standard therapeutic range, or have been taking multiple benzodiazepines simultaneously, inpatient medical detox is strongly worth considering. The risk of severe withdrawal complications is higher, and 24-hour monitoring provides a safety net that outpatient tapering cannot.
People Who Also Drink Alcohol
Alcohol is also a GABA-enhancing drug, and combined benzodiazepine and alcohol dependence produces additive withdrawal risks. Both substances need to be addressed simultaneously under close medical supervision — typically in an inpatient or residential setting.
Frequently Asked Questions
How long does benzodiazepine withdrawal last?
For most people following a gradual taper, acute withdrawal symptoms resolve within a few weeks of the final dose. However, protracted withdrawal symptoms — particularly anxiety, sleep disruption, and cognitive difficulties — can persist for months. The timeline varies significantly based on dose, duration of use, and individual neurobiology.
Can I quit benzodiazepines cold turkey?
No. Quitting benzos cold turkey is medically dangerous and never recommended. Unlike opioid withdrawal (which is extremely unpleasant but rarely fatal), benzodiazepine withdrawal carries a genuine risk of seizures and death. Always taper gradually under medical supervision.
What is the Ashton Manual?
The Ashton Manual is a patient-focused guide to benzodiazepine withdrawal written by Professor Heather Ashton, published at benzo.org.uk. It provides detailed tapering schedules and is widely referenced by patients and clinicians alike, though newer guidelines have updated some of its recommendations.
Is there any medication that makes quitting benzodiazepines easier?
There is no FDA-approved medication specifically for benzodiazepine withdrawal (other than the benzos themselves, used in a taper). However, some physicians use anticonvulsants, beta-blockers, or other supportive medications to manage specific symptoms. None of these is a substitute for a carefully managed taper.
Will I need to be on benzodiazepines forever?
The vast majority of people can successfully discontinue benzodiazepines with appropriate support. Physical dependence is a physiological adaptation — not a life sentence. Many people report that once the acute withdrawal phase passes, their anxiety actually improves, as the medication-induced rebound effect is no longer present.
Conclusion
Quitting benzodiazepines safely requires patience, medical guidance, and a clear plan — but it is absolutely achievable. The 7 steps covered in this guide — consulting your doctor, understanding tapering methods, building a realistic schedule, knowing what symptoms to expect, managing withdrawal without returning to benzos, building a support system, and planning for life after discontinuation — give you a solid framework for the process.
The most important thing to remember is this: never stop abruptly, never go it alone, and never treat your taper timeline as a competition. The slower you go, the higher your chances of getting off these medications for good. With the right team around you and realistic expectations about the timeline, most people can and do successfully end their dependence on benzodiazepines.