Benzodiazepine Tapering Schedule: A Doctor’s Guide
A benzodiazepine tapering schedule done right prevents dangerous withdrawal. A doctor explains the safest methods, timelines, and what to expect.
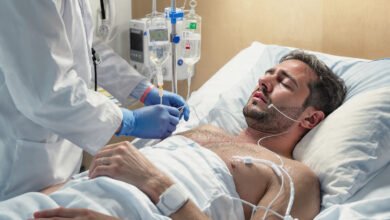
Benzodiazepine tapering is one of the most misunderstood and underestimated processes in modern medicine. Millions of people take benzodiazepines — drugs like Xanax, Valium, Klonopin, and Ativan — for anxiety, insomnia, seizure disorders, or muscle spasms. Many of them have no idea how physically dependent their brains have become until they try to stop.
Stopping benzos cold turkey is not just uncomfortable — it can be life-threatening. Seizures, delirium, and severe rebound anxiety are real risks. That is why a carefully planned benzo taper is not optional. It is medically necessary.
But here is the problem: most people do not get enough guidance. They are handed a prescription for months or years, then told to “just take less.” That is not a plan. A proper benzodiazepine tapering schedule is a structured, individualized roadmap that takes into account which drug you are on, how long you have been taking it, your dose, your age, and your general health.
This guide walks you through everything a doctor would want you to know. From how benzos work and why stopping suddenly is dangerous, to the step-by-step tapering approaches, substitution strategies, and how to manage the symptoms that come up along the way. Whether you are tapering yourself or supporting someone who is, this is the most complete, plain-language breakdown you will find.
What Are Benzodiazepines and Why Does Dependence Happen?
Benzodiazepines are a class of central nervous system depressants that work by enhancing the effect of GABA (gamma-aminobutyric acid), the brain’s primary inhibitory neurotransmitter. When GABA activity increases, the nervous system slows down — anxiety fades, muscles relax, sleep comes easier, and seizures are suppressed.
The catch is that the brain adapts. Over time, GABA receptors downregulate — they become less sensitive and fewer in number — because the drug is doing the job for them. The nervous system compensates by becoming more excitable. This is called neuroadaptation, and it is the biological foundation of benzodiazepine dependence.
This is not a character flaw or a weakness. It is pharmacology. The brain changed in response to a drug, and now it needs time to change back.
Common Benzodiazepines and Their Half-Lives
Understanding half-life is critical for designing a tapering schedule. A longer half-life means the drug leaves the body more slowly, which often produces less severe withdrawal.
| Drug (Brand Name) | Generic Name | Half-Life |
|---|---|---|
| Valium | Diazepam | 20–100 hours |
| Klonopin | Clonazepam | 18–50 hours |
| Ativan | Lorazepam | 10–20 hours |
| Xanax | Alprazolam | 6–12 hours |
| Restoril | Temazepam | 8–20 hours |
| Halcion | Triazolam | 1.5–5 hours |
Short-acting benzodiazepines like alprazolam (Xanax) produce faster, more intense withdrawal symptoms. Long-acting benzodiazepines like diazepam (Valium) taper more smoothly, which is why many physicians use diazepam as a substitution agent during cross-tapering.
Why You Cannot Just Stop: The Risks of Abrupt Discontinuation
Before getting into the benzo tapering schedule itself, it is worth understanding what you are trying to avoid. Abrupt discontinuation of benzodiazepines can trigger a serious, sometimes life-threatening withdrawal syndrome.
Symptoms of abrupt benzodiazepine withdrawal include:
- Rebound anxiety and panic attacks
- Insomnia and vivid nightmares
- Muscle tremors and twitching
- Sweating, rapid heart rate, high blood pressure
- Hypersensitivity to light, sound, and touch
- Seizures (particularly dangerous — can be fatal)
- Delirium (confusion, disorientation, psychosis)
- Nausea and vomiting
The seizure risk is the most critical reason benzodiazepine withdrawal should always be medically supervised, especially for people who have been taking high doses or using them for longer than a few weeks. Benzos and alcohol are two of the only substance classes where withdrawal can kill you.
The 7-Step Benzodiazepine Tapering Schedule
Here is the step-by-step framework used by addiction medicine specialists and psychiatrists when designing a benzo taper protocol. Each step requires individualization — these are principles, not rigid rules.
Step 1: Get a Full Medical Assessment
Before reducing a single milligram, you need a baseline medical evaluation. This means:
- A full medication list (some drugs interact with benzos or affect withdrawal)
- A psychiatric history (anxiety disorders, PTSD, or prior seizures change the approach)
- A physical exam and basic labs
- An honest discussion of your current dose, duration of use, and any previous withdrawal attempts
Do not skip this step. Patients who have had prior withdrawal seizures are at higher risk for seizures in future withdrawals — a phenomenon called kindling. These individuals need closer monitoring and potentially a slower taper.
Step 2: Calculate Your Current Dose in Diazepam Equivalents
To design a safe taper, especially if you are going to switch to a longer-acting drug, you first need to express your current dose in diazepam equivalents. This standardizes the process.
Standard diazepam equivalency table:
| Drug | Equivalent to 10 mg Diazepam |
|---|---|
| Alprazolam (Xanax) | 0.5 mg |
| Clonazepam (Klonopin) | 0.5–1 mg |
| Lorazepam (Ativan) | 1 mg |
| Temazepam (Restoril) | 10–20 mg |
| Diazepam (Valium) | 10 mg |
So if someone is taking 2 mg of alprazolam per day, that is equivalent to approximately 40 mg of diazepam per day. This becomes the starting point for the taper.
(Note: These are approximate equivalencies and can vary between individuals. Always confirm with a prescribing physician.)
Step 3: Choose a Tapering Method
There are three main approaches to benzodiazepine tapering:
Option A: Direct Taper Gradually reduce the dose of the current medication over time. This works well for long-acting benzos like clonazepam or diazepam. Not ideal for short-acting drugs like alprazolam, where small dose changes can produce intense between-dose withdrawal.
Option B: Cross-Taper to Diazepam (Valium) Switch from a short-acting benzodiazepine to diazepam (Valium), then taper the diazepam slowly. This is often recommended in the Ashton Manual, a widely referenced clinical guide developed by Dr. Heather Ashton, a British psychopharmacologist who spent decades studying benzo withdrawal. Learn more about the Ashton Manual here.
The rationale: diazepam’s long half-life creates a natural, built-in buffering effect. The drug self-tapers to some degree, which reduces the severity of inter-dose withdrawal.
Option C: Liquid Titration Using a liquid formulation of the medication allows for very precise, small-increment reductions. This is particularly useful in the final stages of a taper when the dose is already low and small absolute changes represent large percentage changes.
Step 4: Set a Realistic Taper Rate
This is where most people run into trouble — they go too fast.
The general guidance from addiction medicine specialists:
- Reduce by no more than 5–10% of the current dose every 2–4 weeks
- Do not rush. A taper for someone who has been on benzos for several years may legitimately take 12–24 months
- Faster tapers (over weeks to a few months) are appropriate only for people who have been on benzos for a short time at low doses
The 10% rule is widely endorsed in clinical practice. Because you are reducing by a percentage of the current dose rather than a fixed amount, each reduction gets smaller in absolute terms as the dose decreases. This mirrors the shape of the GABA receptor recovery curve, which is not linear.
Example taper using the 10% rule starting from 20 mg diazepam equivalent:
- Week 1–2: 20 mg → 18 mg
- Week 3–4: 18 mg → 16.2 mg
- Week 5–6: 16.2 mg → 14.6 mg
- Week 7–8: 14.6 mg → 13.1 mg
- Continue reducing…
You can see how the pace slows naturally. This is intentional and appropriate.
Step 5: Split the Dose
Short-acting benzodiazepines should always be given in divided doses during a taper. Taking alprazolam once a day leads to inter-dose withdrawal — a mini-withdrawal between doses that causes rebound anxiety, physical symptoms, and drug-seeking behavior. Splitting the daily dose into two, three, or four equal doses taken throughout the day prevents this.
For longer-acting drugs like diazepam or clonazepam, once or twice-daily dosing is usually sufficient.
Step 6: Hold the Taper When Symptoms Flare
A benzo taper is not a straight downward line. It has plateaus, and that is expected and appropriate. If a patient experiences significant withdrawal symptoms at a given dose reduction, the clinical response is to hold the dose — not push through, not reduce further.
Signs that you need to hold:
- Return of significant anxiety, panic attacks, or agoraphobia
- Insomnia severe enough to impair function
- Physical symptoms like tremors, palpitations, or sensory disturbances
- Any neurological symptoms (tingling, zaps, perceptual changes)
Wait until symptoms stabilize — usually a week or two — before attempting the next reduction.
Do not reverse the taper without medical guidance. Going back up on the dose resets part of the process and makes future tapers harder. But if symptoms are severe enough to be dangerous, a temporary dose hold (not increase) is the right call.
Step 7: Manage the Final Stage
The last 20–25% of any benzo tapering schedule is often the hardest. The absolute dose changes are tiny, but paradoxically, many people find this phase the most symptomatic. The receptor system is highly sensitized at this point, and even small reductions can feel significant.
Strategies for the final stretch:
- Slow the taper rate even further (extend intervals to 3–4 weeks per reduction)
- Switch to liquid titration for micro-reductions
- Ensure robust non-pharmacological support is in place (see below)
- Consider short-term adjunctive medications with physician guidance (anticonvulsants, beta-blockers for autonomic symptoms, or low-dose antidepressants for mood support)
The Ashton Manual: A Reference Worth Knowing
The Ashton Manual, formally titled Benzodiazepines: How They Work and How to Withdraw, remains the most comprehensive free clinical guide available for benzo withdrawal. Written by Professor C. Heather Ashton of Newcastle University, it contains sample taper schedules for every common benzodiazepine, explains the pharmacology in plain language, and provides honest, evidence-based guidance on what patients can expect.
It is not a substitute for medical supervision, but it is one of the best educational resources available and is widely used by physicians who specialize in addiction medicine.
Medications That Can Help During a Benzo Taper
While the taper itself is the main treatment, several adjunctive medications can reduce symptom burden. These are not replacements for the taper — they treat specific symptoms while the taper does its work.
Anticonvulsants
- Carbamazepine (Tegretol) and gabapentin have evidence for reducing the severity of benzodiazepine withdrawal symptoms, particularly in the early stages of tapering or during high-risk reductions.
- Valproate is sometimes used, especially when seizure risk is elevated.
Beta-Blockers
Propranolol can reduce the physical symptoms of anxiety — heart racing, trembling, sweating — without affecting the central withdrawal process. It does not prevent seizures and should not be used as a replacement for a proper taper.
Antidepressants
For patients with underlying depression or anxiety disorders that benzos were originally prescribed to treat, starting an SSRI or SNRI during the taper can help manage the mood symptoms that emerge as the benzo is withdrawn. Allow 4–6 weeks for these medications to take effect before expecting results.
Melatonin and Sleep Aids
Melatonin is a reasonable, non-addictive option to support sleep during tapering. Avoid antihistamines (Benadryl, Unisom) for sleep — they have anticholinergic effects that can worsen cognitive symptoms.
Avoid Z-drugs (zolpidem/Ambien, eszopiclone/Lunesta, zaleplon/Sonata). These work on the same GABA-A receptor complex as benzodiazepines and can maintain or worsen dependence.
Protracted Withdrawal Syndrome (PAWS)
Not everyone who completes a benzodiazepine taper feels better immediately once the drug is gone. A significant minority of patients experience protracted withdrawal syndrome (also called post-acute withdrawal syndrome, or PAWS) — a constellation of symptoms that can persist for months or, in some cases, years after the last dose.
Common PAWS symptoms include:
- Persistent anxiety, emotional blunting, or mood instability
- Cognitive difficulties — brain fog, memory issues, word-finding problems
- Insomnia and unusual sleep patterns
- Tinnitus, visual disturbances, or sensory “zaps”
- Burning or tingling sensations in the skin
- Derealization or depersonalization
The mechanism behind PAWS is not fully understood but is believed to involve slow GABA receptor upregulation and compensatory changes in glutamate, serotonin, and other neurotransmitter systems. Recovery from PAWS is real and does happen, but the timeline is highly individual.
For most people, symptoms gradually improve over 6–18 months. The best approach is time, avoidance of other CNS depressants, regular sleep, exercise, and stress management.
Non-Drug Support Strategies
A benzo tapering schedule does not exist in a vacuum. What you do during and after the taper matters enormously for how you feel and how quickly your nervous system recovers.
Cognitive Behavioral Therapy (CBT)
CBT is the gold-standard psychotherapy for anxiety disorders, which are among the most common reasons benzodiazepines are originally prescribed. It helps patients build coping strategies that do not rely on medication. Starting CBT before or during the taper is one of the best investments a patient can make.
Exercise
Regular aerobic exercise has a measurable effect on GABA receptor function and reduces anxiety. Even moderate daily walking can meaningfully support recovery. Exercise is not a luxury during benzo withdrawal — it is part of treatment.
Dietary and Lifestyle Factors
- Avoid alcohol completely during a taper. Alcohol also works on GABA receptors and can worsen dependence and withdrawal symptoms.
- Reduce or eliminate caffeine, which increases nervous system excitability and can worsen anxiety and insomnia during withdrawal.
- Prioritize sleep hygiene — consistent wake times, a dark and cool room, and avoiding screens before bed.
- Eat regular meals. Hypoglycemia (low blood sugar) can trigger or worsen anxiety and mimic withdrawal symptoms.
Peer Support
Organizations like Benzo Buddies and various online communities provide peer support for people going through benzodiazepine tapering. While peer advice should never replace medical care, the social and emotional support available in these communities is genuinely valuable.
Special Populations: Who Needs Extra Caution?
Some patients require extra care in designing a benzo taper schedule:
- Elderly patients: Older adults metabolize benzodiazepines more slowly, are more sensitive to cognitive effects, and face higher fall risk. Tapers should be slower, and diazepam should generally be avoided in this group because of its very long-acting active metabolites.
- Patients with a history of seizures: Prior withdrawal seizures, febrile seizures, or epilepsy increase the risk of seizure during benzo withdrawal. These patients may need inpatient management and anticonvulsant coverage.
- Pregnant patients: Benzo withdrawal during pregnancy carries risks for both mother and fetus. Management should involve both obstetrics and addiction medicine. In many cases, a slow stabilizing taper (rather than aggressive reduction) is the priority.
- Patients on high doses: Someone taking the equivalent of 80–100 mg diazepam per day may require an inpatient medically supervised detox before starting an outpatient taper.
- Patients with co-occurring alcohol use disorder: Alcohol and benzo cross-tolerance complicates management significantly. These patients need specialized dual-diagnosis care.
When to Seek Inpatient or Residential Care
Most benzodiazepine tapers can be done safely in an outpatient setting with a supportive physician. But some situations warrant inpatient or residential care:
- Very high daily doses (over 60–80 mg diazepam equivalent)
- Prior withdrawal seizures
- Concurrent alcohol use disorder
- Severe psychiatric comorbidities (psychosis, active suicidality)
- Lack of a safe and supportive home environment
- Previous failed outpatient taper attempts
Inpatient benzodiazepine detox typically uses diazepam or a long-acting equivalent on a symptom-triggered or fixed-schedule protocol over 5–10 days, followed by transition to an outpatient maintenance taper if needed.
Conclusion
A benzodiazepine tapering schedule is not a one-size-fits-all process — it is a carefully individualized plan that balances the biological reality of GABA receptor recovery with the practical demands of a person’s life. The 7-step framework covered in this guide — from a full medical assessment and diazepam equivalency calculation, through choosing the right tapering method, setting a realistic pace, splitting doses, managing flares, and navigating the final stretch — gives patients and clinicians a clear, evidence-based roadmap.
The key principles are patience, consistency, and medical supervision. Benzos can be tapered successfully, PAWS does resolve for most people over time, and recovery is genuinely possible. But it requires a plan, and it requires not going it alone.